James Maitland has spent the better part of a decade at the intersection of medical robotics and the Internet of Things, championing a vision where the four walls of a hospital no longer define the boundaries of high-quality acute care. His work focuses on integrating sophisticated remote monitoring systems with real-world clinical workflows, a passion born from seeing how technology can bridge the gap between clinical necessity and patient comfort. By examining recent shifts in healthcare delivery, Maitland provides a roadmap for how health systems can transition from traditional inpatient models to more flexible, home-based solutions.
The following discussion explores the clinical efficacy of providing acute care within a residential setting, the geographical disparities that currently limit its reach, and the logistical hurdles of long-term implementation. We delve into why home-based patients often experience fewer complications and lower mortality rates, while also addressing the economic realities of remote monitoring and the legislative support sustaining these programs through the end of the decade.
Recent data indicates that providing acute care in a patient’s home reduces emergency department visits and mortality rates compared to traditional inpatient stays. How do you explain this improvement in safety, and what specific clinical protocols ensure that home-based patients remain more stable than those in hospital wards?
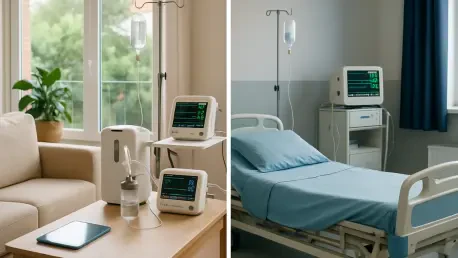
The improvement in safety stems from the elimination of the “hospital environment” stressors that often plague elderly or high-risk patients, such as sleep deprivation from constant floor noise and the disorientation of a sterile, unfamiliar room. When a patient is in their own living room, their baseline physiological state is more stable, which directly contributes to the lower in-hospital mortality rates we are seeing in recent studies. We maintain this stability through rigorous remote monitoring protocols that transmit vitals in real-time to a central command center, allowing clinicians to intervene long before a minor fluctuation becomes a crisis. These protocols include scheduled clinician visits and a continuous digital tether that ensures the patient is never truly “alone,” creating a safety net that feels invisible to the patient but is robust enough to catch early warning signs of deterioration. This proactive stance is exactly why we see a significant decrease in emergency department use within thirty days of discharge, as the transition from acute care to recovery is a seamless glide rather than a jarring handoff.
Most acute home-care programs are currently concentrated in urban centers, leaving rural communities with limited access due to infrastructure and staffing constraints. What logistical strategies could bridge this gap, and how can facilities overcome the lack of high-speed internet or long travel distances for clinicians?
The geographical disparity is stark; currently, of the sixty-eight hospitals leading this charge, eleven of them account for roughly half of all admissions, and every single one of those high-utilizers is located in an urban area. To bridge this gap for rural communities, we have to move away from relying on existing consumer infrastructure and instead deploy “hospital-in-a-box” solutions that include cellular-based hot spots and satellite-linked monitoring tools to bypass poor local internet. Logistically, we can address the long travel distances by utilizing a hub-and-spoke staffing model where local paramedics or specialized nurses are stationed in rural clusters, reducing the transit time for the “boots on the ground” while the primary physician consults via high-definition video. It is disheartening to see that while the Northeast and South are seeing concentrated growth, the West remains largely underserved in this sector, particularly among high-utilization hospitals. Overcoming this requires a targeted investment in mobile health units that can act as roaming command centers, ensuring that a patient’s zip code doesn’t dictate their access to this safer, more comfortable tier of medicine.
While home-level care decreases certain complications, 30-day readmission rates remain similar to traditional stays, and the overall duration of care is often longer. Why does the recovery timeline shift in a home environment, and what metrics should administrators prioritize to manage these longer treatment cycles?
The recovery timeline shifts because home-based care often prioritizes a gradual, functional recovery over the “stabilize and discharge” urgency found in over-crowded hospital wards. In a hospital, the goal is often to free up the bed for the next acute case, whereas at home, the “bed” is already where the patient lives, allowing for a longer tail of supervised care that results in minor decreases in total healthcare costs despite the extended duration. Administrators need to stop looking at “length of stay” as the primary efficiency metric and instead focus on “total cost of the acute episode” and “patient functional independence” scores. Even though 30-day readmission rates currently show no significant difference between the two cohorts, the quality of life during those thirty days is vastly superior for the home-based patient. By managing these longer cycles with automated scheduling and AI-driven triage, we can ensure that the extended care period remains cost-effective while providing a more thorough healing process that eventually reduces the burden on the broader healthcare system.
With federal reimbursement for home-based acute care extended through September 2030, many health systems are deciding whether to invest in these programs. What are the primary financial risks during this expansion, and how should hospitals structure their remote monitoring and staffing to justify the long-term investment?
The primary financial risk lies in the “middle ground” of adoption, where a hospital has enough patients to incur high overhead costs for technology and staffing but not enough volume to achieve the economies of scale seen in the top eleven high-utilizer programs. With the CMS extension through September 2030, hospitals now have a clear six-year runway to build these programs, which should alleviate some of the “sunset anxiety” that previously hindered capital investment. To justify the long-term expenditure, systems should structure their staffing around hybrid roles where clinicians manage both virtual and physical rounds, maximizing their utility across a larger patient base. Integrating IoT sensors that automate routine data collection—like continuous pulse oximetry and movement tracking—can also reduce the labor-intensive nature of monitoring, making the program more resilient to the staffing shortages that currently plague the industry. By viewing this as a long-term capacity management strategy rather than a temporary pilot, hospitals can free up their high-acuity inpatient beds for surgical cases and intensive care, which ultimately drives higher revenue for the physical facility.
Patients treated at home appear less likely to develop hospital-acquired infections or require escalation to intensive care. How does the physical environment of a residence contribute to these lower infection rates, and what are the step-by-step procedures for identifying when a home patient truly needs an ICU transfer?
The physical environment of a home is naturally devoid of the multi-drug resistant organisms that frequently colonize hospital surfaces and ventilation systems, which is the primary reason we see such a dramatic drop in hospital-related complications. When a patient isn’t sharing a hallway with dozens of other acutely ill individuals, the chain of transmission for infections like MRSA or C. diff is effectively broken at the front door. However, the protocol for identifying the need for an ICU transfer must be incredibly precise: it begins with continuous telemetry that triggers an immediate alert if vitals cross a specific acuity threshold, followed by a rapid video assessment by a critical care physician. If the physician determines that the patient requires interventions that cannot be safely performed at home—such as mechanical ventilation or continuous vasopressor support—a pre-arranged medical transport is dispatched immediately. This tiered approach ensures that while we keep patients away from the risks of the hospital ward, we maintain a “fail-safe” mechanism that moves them to a higher level of care the moment their clinical trajectory suggests a need for intensive resources.
What is your forecast for hospital-at-home programs?
My forecast is that hospital-at-home will evolve from a niche “alternative” into a standard tier of the American healthcare continuum, eventually accounting for 10% to 15% of all acute admissions as the 2030 deadline approaches. We will see a massive push toward “technological equity,” where the federal government and private payers collaborate to subsidize the broadband and hardware necessary to bring these programs to the rural West and Midwest. As the data continues to prove that we can achieve lower mortality and fewer complications at a lower total cost, the pressure from both patients and insurers will make it nearly impossible for major health systems to remain on the sidelines. I expect to see the “high-utilizer” group expand from just eleven urban hospitals to hundreds of facilities nationwide, fueled by a new generation of “virtualist” physicians who specialize exclusively in managing high-acuity patients through a digital lens. Ultimately, the home will no longer be seen as a place where care ends after discharge, but as the primary site where healing begins for the most common acute conditions.