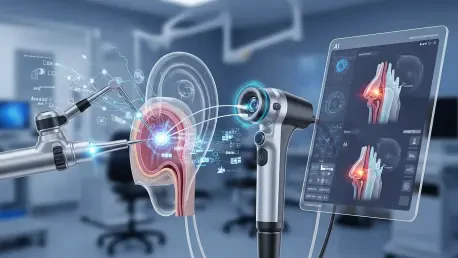
Relentless patient volumes, tighter operating room timelines, and rising expectations for safer, faster care have pushed ear, nose, and throat practice into a technology-first chapter that links diagnostics and treatment more tightly than ever before. Momentum has coalesced around AI-augmented imaging, real-time navigation, and robotics that promise to standardize quality and extend advanced ENT capabilities into outpatient settings. The market effects have been tangible: new approvals, clinic-ready platforms, and broader reimbursement are enabling providers to integrate tools that compress diagnostic timelines and reduce variability in surgical outcomes. This shift is not a short-lived upswing. It reflects structural forces—aging demographics, expanding access in emerging economies, and a sustained pivot to minimally invasive care—that anchor growth through 2034.
Market Momentum and Scale
Size and Growth to 2034
The ENT Devices Market has been tracking a steady expansion, with projections pointing from about US$22.95 billion in 2025 to roughly US$37.92 billion by 2034, a compound annual growth rate of 5.8% during 2026–2034 that aligns with consistent clinical need rather than cyclical spikes. Growth has been underpinned by rising baseline demand for hearing, sinus, and laryngology care alongside modernization of clinical workflows. Hospitals, ambulatory surgery centers, and specialty clinics continue to expand installed bases of endoscopes, imaging suites, and navigation systems, creating repeatable upgrade cycles. That foundation supports device makers as they layer connectivity and AI into familiar form factors. In effect, the market’s scale has been reinforced by design decisions that enable stepwise adoption rather than wholesale replacements.
Beyond headline numbers, the market’s composition has favored platforms with interoperable software and fleet-level management, which reduce downtime and ease cybersecurity oversight. Imaging vendors have emphasized 4K and 3D visualization with noise reduction and dynamic range tuning suited to delicate ENT anatomy, marrying hardware gains with AI-assisted enhancement. On the procedure side, balloon sinus dilation and powered instrumentation have broadened case selection for minimally invasive approaches, shifting some interventions to outpatient suites. Those workflow efficiencies have resonated with payers focused on value per episode of care. As a result, capital deployment has tilted toward systems that promise faster turnover, lower complication rates, and predictable maintenance, attributes that make five- to seven-year refresh cycles easier to justify.
Clinical and Access Drivers
Demand has risen on the back of three converging realities: more patients with chronic ENT conditions, a decisive move toward earlier diagnosis, and a preference for less invasive treatment. Hearing loss screening has moved upstream in primary care and occupational health, while sinusitis pathways now often begin with high-definition endoscopy and point-of-care imaging, enabling targeted medical therapy or timely dilation. AI has supported this shift with real-time lesion detection in rhinolaryngoscopes that flags suspicious tissue and standardizes documentation. In parallel, aging populations in North America and Europe have amplified caseloads for cochlear and bone conduction implants, encouraging investments in surgical navigation and intraoperative monitoring that help safeguard critical structures.
Access trends have mattered just as much. Asia Pacific systems have been modernizing ENT suites with cloud-connected scopes and portable endoscopy towers that ease deployment across urban and semi-urban networks, while reimbursement reforms in select markets have recognized outpatient sinus and laryngology procedures. Remote consultation and imaging review have improved triage for underserved regions by allowing specialists to guide workups before referral, which shortens time to diagnosis. These structural gains have dovetailed with rapid training cycles supported by simulation and digital curricula, helping more clinicians perform advanced procedures safely. The cumulative effect has been a higher baseline of diagnostic precision and procedure eligibility, which sustains equipment utilization and replacement demand.
Tech Shifts Redefining ENT
AI, Imaging, Navigation, and Robotics
Three technology vectors have shaped product roadmaps and purchasing criteria. First, AI-integrated diagnostics have matured from retrospective analysis to live decision support; AI-assisted rhinolaryngoscopes now highlight microvascular patterns and textural anomalies in real time, aiding early detection of dysplasia in outpatient visits. Second, next-generation imaging and navigation fuse high-definition visuals with CT or cone-beam datasets, anchoring the endoscopic view to anatomical landmarks with submillimetric guidance. Vendors have focused on latency, registration accuracy, and ergonomic overlays that reduce surgeon cognitive load. Third, robotics has advanced in scope and precision, integrating tremor filtration and constrained workspaces suited to transoral access, with platforms designed to harmonize with existing imaging and navigation stacks.
Regulatory momentum has reinforced clinical confidence. Approvals for upgraded navigation modules and imaging processors signaled readiness for broad integration, while post-market studies documented reductions in operative time variability when navigation and AI-based mapping were used together. Companies have moved accordingly. Olympus emphasized visualization ecosystems that align optical performance with AI firmware updates. Stryker and Medtronic advanced navigation compatibility across ENT and cranial workflows, prioritizing shared workstations and software continuity. Ambu pushed single-use endoscopes with cloud reporting to mitigate cross-contamination and speed turnover. On the implant side, MED-EL focused on surgical planning and telemetry that feed back into post-activation tuning, linking the operating room to rehabilitation.
Measurable Clinical and Operational Gains
Clinical benefits have moved from promise to measurable effect sizes in core use cases. For chronic rhinosinusitis, pairing HD endoscopy with AI-aided image enhancement improved mucosal assessment sensitivity, enabling earlier escalation to balloon dilation when conservative therapy failed. In laryngology, real-time pattern recognition helped flag suspicious lesions for biopsy in the same visit, reducing follow-ups and patient anxiety. Surgeons reported steadier workflows in skull base and complex sinus cases when navigation overlays synchronized tightly with the endoscopic scene, which reduced the time spent reorienting after bleeding or partial obstruction. The combined impact has been fewer false negatives, firmer indications for intervention, and more predictable outcomes across mixed-experience teams.
Operationally, integrated platforms reshaped the economics of ENT suites. Robotics paired with navigation reduced setup guesswork and instrument exchanges, shaving minutes that compound across daily schedules. Single-use scopes curtailed reprocessing queues and infection risk, while cloud-linked documentation automated coding support and quality reporting. These efficiencies mattered to payers and health systems aligning incentives around day-case surgery and shorter lengths of stay. Yet constraints persisted: training curves for robotic transoral approaches, capital budgeting for multi-modality stacks, and the need for secure data pathways in distributed networks. Addressing these, leading centers established proctoring hubs, negotiated enterprise software licenses, and standardized network segmentation. Taken together, the path forward called for phased adoption plans, cross-specialty governance for imaging assets, and outcome tracking tied to financing models that rewarded precision and speed.