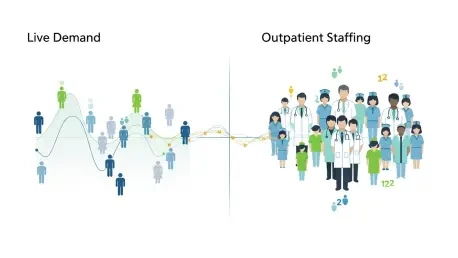
Outpatient backlogs no longer hinge on appointment volume alone; the chokepoint now is synchronizing the right clinician, at the right site, at the right minute as demand whipsaws across networks and schedules fracture under cancellations, no-shows, and late add-ons. That operational gap has become the decisive arena for access, throughput, and cost, and it explains why investment has shifted from passive analytics to agentic systems that coordinate work. UnityAI, a Nashville startup, sits squarely in this trend with StaffOps, an agentic platform built to align staffing supply with real-time demand signals across multi-site ambulatory care.
The Operational Problem Agentic AI Is Built to Solve
Why Static Schedules Break Under Volatile Demand
Templates assume steady patient flow; real clinics live with churn. Same-day cancellations, uneven site volumes, and end-of-day add-ons scramble coverage, leaving one clinic overrun while another idles. The result is degraded access, lower throughput, and wasteful labor spend that compounds week after week.The root issue is structural: appointment signals remain disconnected from staffing actions. Without a closed loop, leaders cannot translate live demand into immediate redeployment, and lost capacity never returns to the schedule.
Two-Sided Operations: Staffing and Patient Access as One System
A provider’s product is time-with-clinician at a place and time, so access and staffing form a single operating system rather than parallel lanes. When access conditions change, staffing must flex; when staffing shifts, access must update.Design follows from that premise. The only durable solution unifies access management and labor operations on shared, real-time data so supply and demand can rebalance continuously across the day.
UnityAI StaffOps: Platform Overview and Core Capabilities
Data Foundation and Integrations
StaffOps integrates with EHRs for live appointments, confirmations, reschedules, cancellations, and throughput, then fuses that stream with HR data for rosters, credentials, scope, site eligibility, language skills, and preferences.This creates a shared operating picture that dissolves the access–staffing split and exposes the true constraints driving daily coverage choices.
Dynamic Optimization and Multi-Site Orchestration
Optimization engines evaluate licensure, role requirements, site coverage, language, and preferences to propose mathematically sound staffing moves.Crucially, the platform treats clinics as one networked system, surfacing cross-site trades and reassignments that raise throughput without raising headcount, while manager tools streamline exceptions.
Agentic Workflows With Human-in-the-Loop Control
Voice and SMS agents handle routine call-offs, swaps, and PTO approvals, cutting coordination time from hours to minutes.As demand shifts throughout the day, StaffOps proposes proactive coverage adjustments and executes outreach, while humans adjudicate edge cases and ensure policy adherence.
Staff Experience and Self-Service
A single interface lets clinicians and support staff request or release shifts and submit PTO with clear visibility into rules and outcomes.Faster decisions and transparent logic reduce administrative drag, supporting retention and mitigating burnout by making schedules predictable and fair.
Market Momentum and Adoption Landscape
Growth Signals and Adoption Trends
Health systems are moving from insight to action, funding orchestration layers that close the loop between EHR and HR in real time. KLAS, Gartner, and McKinsey analyses echo the shift toward AI in workforce operations, while provider associations and policymakers emphasize access and throughput.Integration-first strategies now serve as table stakes; without live connectivity, “dynamic staffing” remains a slide, not a system.
Real-World Traction and Use Cases
StaffOps is live at roughly 120 outpatient sites across multiple organizations, following an early path through front-office agents for scheduling, confirmations, intake, and follow-up. The pivot to multi-site ambulatory operations accelerated impact by meeting structured, operations-focused networks.Representative scenarios include rebalancing after same-day cancellations, late-day add-ons via agentic outreach, language-matched coverage for defined cohorts, and cross-role coverage within licensure and scope.
Expert and Industry Perspectives on Agentic Operations
Operators endorse human-in-the-loop exception handling for trust, safety, and compliance, and workforce leaders stress that self-service plus transparent, fair rules drives adoption. Technology leaders point to the combination of optimization and natural-language interaction to compress coordination cycles.Health system priorities are pragmatic—access, throughput, and labor productivity—while governance focuses on credentialing, union terms, and equitable assignment logic. Suggested stakeholders include COOs, nursing workforce leaders, ambulatory operations directors, and AI safety committees.
Implementation Realities, Limits, and Risks
Change Management and Governance
Effective rollouts start with codified policies for reassignments, coverage rules, and escalation paths. Cross-functional alignment across operations, HR, compliance, and clinic leadership prevents whiplash in the field.Training and clear communications secure frontline acceptance by demystifying how recommendations are made and when humans override them.
Data Quality, Interoperability, and Regulatory Constraints
EHR variation, credentialing accuracy, and update latency can erode optimization quality. Union agreements, state scope-of-practice rules, and scheduling regulations bound what is permissible.Privacy, security, and audit trails for voice and SMS workflows must be rigorous, since staffing data intersects with protected patient and employee information.
Evidence and Measurement
Programs need explicit baselines: cancellation rates, fill rates, overtime and agency spend, visit throughput, and wait times. A/B or phased rollouts attribute lift to specific interventions.Transparent reporting of gains and gaps feeds continuous tuning of optimization constraints and message strategies.
Strategic Trajectory and Industry Implications
Roadmap to Semi-Autonomous Labor Operations
The arc points to agents that coordinate both demand and supply with minimal manual effort. Closed-loop execution—detect signal, recommend plan, communicate changes, confirm coverage—turns staffing into a living system.Guardrails for fairness, fatigue, and equity remain embedded, ensuring productivity does not compromise clinical quality or staff well-being.
Cross-Specialty Scalability in Ambulatory Networks
Radiology, dental, behavioral health, substance use treatment, and primary care share variability patterns that benefit from multi-role, multi-site orchestration.As networks standardize policies, the same backbone can rebalance staff across service lines without rebuilding logic for each clinic.
Outcomes—Upsides and Watch-Outs
Potential gains include fewer preventable cancellations, higher throughput, optimized labor costs, and improved staff experience.Risks involve misaligned incentives, alert fatigue, opaque algorithms, and local policy conflicts; mitigations include transparent rules, auditability, opt-outs, and continual calibration.
Summary and Call to Action
Agentic AI redefined operations by turning data into coordinated action, and StaffOps exemplified that shift by unifying EHR and HR data to align staffing with live demand across sites and roles. Early deployments demonstrated feasibility in multi-site outpatient networks while reinforcing that governance, data quality, workforce trust, and measurable outcomes set the adoption curve.Providers considering this path could start by mapping demand signals and staffing workflows, assessing integration readiness, piloting agentic coverage with explicit metrics and guardrails, and establishing a cross-functional governance cadence. Done well, the move positioned organizations to expand access, compress cycle times, and manage labor with precision at network scale.