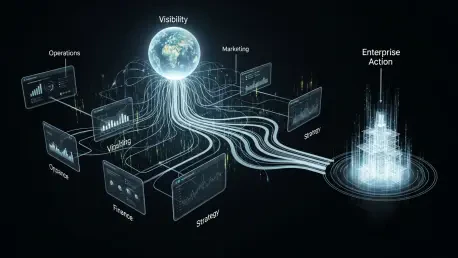
Hallway waits, full EDs, and unanswered pages signal a deeper issue: visibility without coordinated action slows care when minutes matter, and this guide shows how to turn real-time awareness into reliable, enterprise-wide decisions that lift throughput, safety, and experience. It defines a practical, step-by-step path to build intelligent care—an operating model that aligns people, workflows, and technology so information triggers timely action across settings.
This guide helps leaders and operators replace siloed tools with real-time orchestration. Readers will learn how to design a shared vision, stand up an operations hub, connect virtual care and smart hospital signals, and apply AI where readiness exists. The outcome is a coordinated system that anticipates demand, smooths transitions, and reduces the effort required to deliver consistent care.
Why Real-Time Orchestration, Not More Tools, Now Defines Care Performance
Healthcare delivery now unfolds as a web of concurrent decisions: bed placement depends on discharge timing, consults hinge on transport readiness, and virtual touchpoints change staffing needs. When these events are managed in isolation, the enterprise lurches from one constraint to another, and the patient journey fragments.
More dashboards or apps do not solve the flow problem if data and accountability remain scattered. Intelligent care reframes the challenge as orchestration, aligning teams around shared signals and standard triggers so the right person receives the right prompt at the right time—and can act with confidence.
From Digital Islands to Enterprise Flow: What Changed and Why It Matters
Years of investment delivered visibility inside departments but rarely across them. As a result, even basic questions—how many discharges are imminent, which units can flex capacity, what beds will open by shift change—often lack a single, trustworthy answer.
Teams bridge the gap with calls, chats, and workarounds that exhaust attention and still arrive too late. The emerging consensus is clear: set strategy before buying tools, connect existing assets for action, and shift from point fixes to enterprise coordination that operates in real time.
How to Build Intelligent Care as an Operating Model
Step 1: Align on a Shared Vision Anchored to the Patient Journey
Agree on end-to-end outcomes—throughput, experience, and safety—and define governance that owns flow across settings. Tie success to patient-journey moments, not departmental metrics, so tradeoffs become explicit and shared.
Tip: Co-Design the Future State With Frontline Teams and Operations Leaders
Bring bedside experts and flow leaders into design to ensure goals reflect reality and changes fit daily practice.
Watch-out: Avoid Tech-First Roadmaps That Outpace Workflow Readiness
Sequence enablement to match process maturity; premature tooling hardens bad habits and erodes trust.
Step 2: Map Current State and Pinpoint Friction in Patient Flow
Trace admissions, transfers, and discharges as they actually occur, then quantify delays, rework, and handoff gaps. Make bottlenecks visible so improvement focuses on constraints with the greatest system impact.
Insight: Start Where Variability and Impact Are Highest (ED, Periop, ICU)
Target volatile nodes first; stabilizing these flows unlocks capacity enterprise-wide.
Practice: Use Time-Stamped Data and Shadowing to Validate Assumptions
Pair data with on-the-ground observation to separate signal from anecdote and reveal hidden queues.
Step 3: Create a Shared, Real-Time Data Layer and Signal Standards
Unify EHR, bed, staffing, and device data into a governed, live view. Define ownership and service levels so updates are timely, complete, and actionable across teams.
Tip: Normalize Status Signals (Ready-to-Discharge, Bed-Clean, Transport-Requested)
Standard names and states reduce confusion and power consistent triggers and alerts.
Watch-out: Don’t Build Custom Feeds That Break Under Change; Use Interoperable Standards
Favor scalable interfaces and event-driven patterns to preserve agility as systems evolve.
Step 4: Stand Up an Operations Hub to Orchestrate Capacity and Flow
Establish a command capability that forecasts demand, allocates beds, and coordinates transitions. Use playbooks that translate signals into decisions, then measure outcomes in near real time.
Example: Predict Next-12-Hour Bed Needs by Unit and Admit Source
Blend arrivals, discharges, and staffing to pre-position capacity where demand will land.
Practice: Pair Hub Roles With Unit-Based “Air Traffic Controllers” for Local Action
Central foresight works best when matched with empowered unit leads who can act immediately.
Step 5: Embed Virtual Care and Smart Hospital Signals at the Bedside
Extend reach with virtual nurses, remote monitoring, and connected devices that close information gaps. Route insights directly into workflows so action happens without extra hunting.
Tip: Route Early Deterioration Alerts to Virtual Teams for Rapid Response
Virtual coverage accelerates recognition and intervention, especially during off-hours.
Insight: Use Automation for Routine Updates (Bed Clean Complete, Patient Transport ETA)
Automated signals remove manual chasing and keep everyone aligned to the latest state.
Step 6: Automate Decisions and Triggers With AI Where Readiness Exists
Apply AI to forecasting, prioritization, and exception detection, keeping humans in the loop for oversight. Start with use cases that complement current practice and expose rationale.
Practice: Start With Explainable Models for Discharge Prediction and Staffing
Transparent drivers build confidence and speed adoption across clinical and operational teams.
Watch-out: Align Algorithms With Policy and Equity Safeguards
Audit performance across populations and codify guardrails to prevent unintended bias.
Step 7: Drive Adoption, Measure Results, and Scale What Works
Create playbooks, training, and feedback loops that reinforce new behaviors. Track throughput, LOS, and experience, and use findings to refine triggers, staffing, and escalation paths.
Tip: Publish Daily “Flow Health” Dashboards for Shared Accountability
Visible metrics focus attention and sustain momentum across shifts and sites.
Insight: Reinforce Behaviors With Lightweight, In-Workflow Nudges, Not Extra Steps
Design prompts that fit naturally so compliance stays high and fatigue stays low.
Quick Recap of the Intelligent Care Playbook
- Align on a patient-journey vision and governance, then map real flow and quantify friction to target the true constraint.
- Build a shared, real-time data layer with standard signals, stand up an operations hub, and connect virtual care and smart telemetry at the bedside.
- Layer AI and automation for forecasts and triggers, and institutionalize adoption, measurement, and scaling to lock in gains.
Where This Model Scales Next: Trends, Use Cases, and What to Watch
The field is pivoting from point fixes to enterprise coordination, unlocking more value from existing assets and enabling hybrid teams that blend virtual and in-person expertise. This approach supports system-wide bed brokerage, tighter perioperative-to-ICU handoffs, and reliable hospital-at-home logistics.
Next, expect staffable capacity models, ambient data capture that reduces documentation burden, and closed-loop tasking across partners. Challenges remain—change fatigue, data quality, equity in automation, and incentive alignment—but disciplined orchestration makes them manageable and measurable.
Make Visibility Actionable: Start Small, Prove Value, Then Scale
This guide translated shared awareness into steps that produced timely, coordinated decisions and better journeys. The most effective starts focused on one high-impact flow, connected existing data, and operationalized decisions through an operations hub, then expanded as results stacked up.
Moving forward, leaders could choose a pilot pathway, convene a cross-functional team within the next month, and stand up the first shared, real-time view. Early wins then became the platform for AI-enabled triggers, broader virtual coverage, and durable governance that protected performance gains.