The rapid integration of sophisticated mechanical assistance into the modern operating room has fundamentally altered the trajectory of patient care and surgical education across the globe. While major metropolitan centers often receive the bulk of attention for technological breakthroughs, a non-profit medical center in Yuma, Arizona, known as Onvida Health, is currently redefining how these complex systems are taught and mastered. This shift signifies a departure from traditional apprenticeship models, moving instead toward highly specialized training hubs that leverage the precision of robotic interfaces to minimize human error and accelerate recovery times. By achieving a prestigious designation as a premier training site, this facility has positioned itself as a critical node in a national network of medical excellence, drawing practitioners from major healthcare markets to a city that was once considered geographically isolated. The emergence of such a high-caliber program in the Southwest underscores a broader trend where clinical expertise and technological investment are becoming decentralized, allowing smaller communities to lead the charge in defining the national standard for minimally invasive procedures.
This institutional evolution is not merely a localized achievement but a significant milestone in the broader landscape of American healthcare delivery and surgical innovation. By serving as an epicenter for peer-to-peer education, Onvida Health facilitates a unique environment where surgical teams can observe real-time applications of robotic technology in a clinical setting. This hands-on observation is crucial for surgeons transitioning from traditional laparoscopic methods to the more intuitive, console-driven interfaces that define modern medicine. The program’s success is built upon a foundation of significant infrastructure growth, moving from a modest setup to a robust fleet of seven advanced systems in a remarkably short period. This expansion allows the facility to handle a diverse range of cases, from routine gallbladder removals to intricate hernia repairs, while simultaneously hosting visiting professionals. The ripple effect of this training model ensures that the benefits of precision robotics—such as reduced blood loss and shorter hospital stays—are disseminated far beyond the borders of Arizona, ultimately improving the quality of care for patients across the entire country.
Institutional Growth and Technological Integration
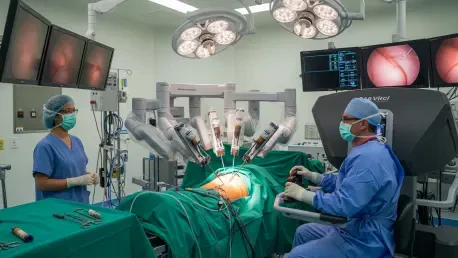
The transition from conventional surgical methods to a fully integrated robotic program requires a massive commitment to both capital investment and specialized human capital. Since 2026, Onvida Health has aggressively expanded its capabilities, scaling its infrastructure to include seven state-of-the-art robotic systems that serve as the backbone of its surgical department. Under specialized leadership, the hospital has successfully completed over 2,000 procedures, proving that high-volume throughput and high-quality outcomes can coexist in a non-profit setting. The technology functions through a sophisticated interface where the surgeon sits at a dedicated console, manipulating controls that translate their hand movements into precise actions by robotic arms. These arms, equipped with micro-instruments, enter the body through tiny incisions that are significantly smaller than those required in traditional open surgery. This level of precision allows for a degree of maneuverability that the human hand alone cannot achieve, particularly in the confined spaces of the abdominal or thoracic cavities, which is essential for complex reconstructive work.
Beyond the hardware itself, the success of a robotic surgery program hinges on the meticulous synchronization of the entire operating room staff and the rigorous maintenance of sterile protocols. Every procedure involves a detailed setup phase where surgical technologists must prepare the robotic arms with sterile drapes, acting as specialized barriers to ensure the integrity of the surgical field. This preparation is a critical component of the training curriculum offered at the facility, as visiting teams must learn not only how to operate the console but also how to manage the logistical complexities of a robotic-ready room. The efficiency of these “behind-the-scenes” maneuvers often determines the overall safety and speed of the operation. By mastering these workflows, the Yuma-based team has created a blueprint for operational excellence that other hospitals strive to replicate. This focus on the holistic surgical environment, rather than just the robotic interface, ensures that the transition to advanced technology is seamless, safe, and sustainable for healthcare institutions looking to modernize their surgical offerings over the next several years.
Educational Impact and Future Standards
The designation of a local hospital as a national training epicenter signals a fundamental shift in how the medical community approaches the dissemination of specialized knowledge. By hosting surgical teams from distant states like Washington and California, the program in Yuma is effectively setting the benchmark for how minimally invasive techniques should be practiced and taught. This peer-to-peer education model is increasingly vital as surgical technology becomes more complex and the learning curve for new systems grows steeper. Practitioners traveling to these observation sites gain insights that cannot be gleaned from textbooks or simulators alone; they witness the nuances of patient positioning, the communication between the surgeon and the bedside assistant, and the management of unexpected intraoperative challenges. This immersive experience is essential for building the confidence and competence required to implement similar programs in their home institutions. As more surgeons achieve proficiency through this epicenter model, the standard of care across the United States is elevated, making advanced robotic surgery a more accessible option for a larger segment of the population.
Looking ahead, the role of specialized training hubs will only become more prominent as the next generation of robotic platforms and artificial intelligence integration enters the clinical space. The groundwork currently being laid by institutions like Onvida Health provides a framework for how these future technologies can be ethically and effectively integrated into patient care. The emphasis on high-volume experience and transparent outcome tracking creates a data-rich environment that can inform future clinical guidelines and best practices. As surgical medicine continues to move toward a more digitized and automated future, the human element—the expert training and the shared wisdom between veteran and novice surgeons—remains the most critical factor in ensuring patient safety. The continued success of the Yuma program serves as a reminder that innovation is not just about the machines themselves, but about the collaborative systems designed to master them. By prioritizing comprehensive training and technological investment, the medical community can ensure that the benefits of the robotic revolution are realized consistently across diverse healthcare settings, regardless of their size or location.
Actionable Strategies for Clinical Excellence
The trajectory of surgical medicine now demands a proactive approach to technology adoption that prioritizes structured mentorship and long-term infrastructure planning. Healthcare administrators should focus on developing localized centers of excellence that can serve as regional training hubs, reducing the need for clinical staff to travel long distances for specialized certification. By investing in a fleet of machines rather than a single unit, hospitals can ensure enough case volume for surgeons to maintain high proficiency levels, which is a key driver of positive patient outcomes. Furthermore, the integration of surgical technologists into the core training curriculum is essential; the logistical prep work is just as vital as the surgeon’s movements at the console. Future efforts must also include a commitment to transparent data sharing regarding recovery times and complication rates to further validate the efficacy of robotic-assisted methods over traditional techniques. This evidence-based approach will be crucial for securing continued funding and support from both non-profit boards and government health agencies.
As the industry moves toward 2028 and beyond, the focus must shift from simply acquiring technology to perfecting the educational pathways that support it. Medical institutions should look to establish formal partnerships with technology developers to create standardized observation protocols that can be scaled across different hospital systems. Encouraging a culture of continuous learning where senior surgeons routinely observe and mentor their peers will foster an environment of safety and innovation. Additionally, hospitals should explore the use of tele-proctoring and remote observation tools to supplement in-person visits, allowing for a more flexible and continuous exchange of surgical expertise. By adopting these strategies, the medical community can ensure that the transition to a more automated and precise surgical landscape is managed with clinical rigor. Ultimately, the goal is to create a decentralized network of high-performing centers that can provide every patient, regardless of their geographic location, access to the highest standard of minimally invasive care. The work currently performed in Yuma provides the necessary evidence that this model is not only possible but highly effective for the modern era.