Modern healthcare systems are operating under an unprecedented level of strain as they attempt to balance the rising demand for complex surgical interventions with increasingly limited institutional resources. At the heart of this struggle is the surgical suite, a high-stakes environment where even a minor delay can cascade into a series of logistical failures that impact patient safety and provider morale. MUSC Health, a prominent academic medical center located in South Carolina, has taken a decisive step toward resolving these systemic challenges by integrating ambient artificial intelligence and advanced predictive analytics into its perioperative workflows. This transition represents a fundamental shift away from the traditional reliance on manual, often subjective data entry toward a high-fidelity, automated tracking system that provides a definitive “ground truth” for hospital operations. By establishing an objective digital record of every movement within the operating room, the institution is not only optimizing its physical capacity but also rebuilding the trust between administrative leadership and clinical teams.
Overcoming Data Subjectivity and Operational Constraints
Bridging the Visibility Gap in the Operating Room
Before the current era of automated oversight, MUSC Health found itself grappling with a significant lack of transparency regarding the utilization of its primary surgical assets. The main operating rooms were functioning at near-maximum capacity, which left almost no margin for error or unexpected disruptions. When delays inevitably occurred, there was no centralized, objective method to determine exactly where the breakdown had happened, leading to a culture of reactive management. The lack of a reliable data stream meant that any attempt to improve efficiency was met with resistance, as there was no consensus on what the problems actually were. This visibility gap made it nearly impossible to implement strategic changes that would stick, as the underlying metrics were seen as incomplete or misinterpreted by those on the front lines.
The administrative burden of manual data entry further complicated this visibility issue, as clinicians were often forced to prioritize patient care over the meticulous logging of timestamps in the Electronic Health Record. This reality created a cycle of skepticism; surgeons and nursing staff frequently questioned the accuracy of performance reports, viewing them as flawed reflections of their actual clinical efforts. Without a shared, trusted understanding of how time was being spent, discussions about operating room turnover or case duration often devolved into anecdotal arguments rather than data-driven strategy sessions. Consequently, the institution needed a way to capture the granular reality of the surgical environment without adding to the cognitive load of its providers, ensuring that every second of room time could be accounted for and optimized through verifiable evidence.
Confronting the Limitations of Manual Documentation
Reliance on manual documentation within the surgical suite often results in a phenomenon known as “timestamp drift,” where the recorded time of an event differs significantly from its actual occurrence. At MUSC Health, this discrepancy was not merely a clerical nuisance but a structural barrier to efficient resource allocation and future planning. Because the data in the electronic records was often entered retroactively, it failed to capture the nuances of room preparation, anesthesia induction, or the specific reasons behind a prolonged turnover. This lack of detail meant that leadership could see that a room was idle, but they could not discern whether that idleness was due to a cleaning delay, a staffing shortage, or a scheduling misalignment. This ambiguity prevented the surgical department from maximizing its throughput during peak hours.
Furthermore, the subjective nature of manual entry meant that data was often influenced by the individual perceptions and priorities of the staff member logging the information. This created a fragmented view of the perioperative process, where different departments might have conflicting records of the same event. To move forward, the health system required a paradigm shift toward “ground-truth” information—objective data captured in real-time by an impartial observer. By moving away from human-dependent logging, MUSC Health aimed to eliminate the friction caused by untrusted metrics and replace it with a transparent, automated system that would serve as the definitive record of truth. This shift was essential for identifying the precise bottlenecks that were limiting the institution’s ability to serve a growing patient population effectively.
Implementing Automated Intelligence and Stakeholder Alignment
Integrating Ambient AI into Clinical Workflows
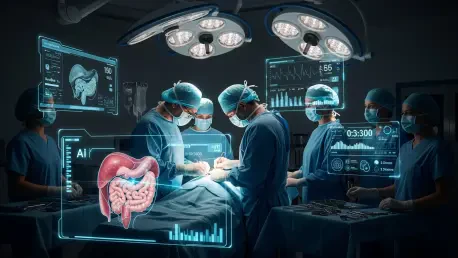
To address these deep-seated operational challenges, MUSC Health partnered with a technology vendor to deploy an ambient AI platform that integrates directly into the existing surgical environment. This technology functions through passive observation, utilizing artificial intelligence to automatically detect and log critical milestones throughout the surgical day. Unlike traditional software that requires active input, this system operates in the background, capturing data on room entry, anesthesia start, surgical incision, and the various stages of the turnover process. By automating these logs, the platform provides a level of detail that was previously unattainable, allowing the perioperative team to view a live, high-fidelity timeline of every active operating room across the entire facility.
The implementation of this technology has provided immediate dividends in terms of real-time situational awareness for the entire clinical team. Charge nurses and surgical coordinators now utilize live dashboards that offer predictive updates on case completion times, enabling them to proactively adjust staffing levels and room assignments. If a procedure is running longer than expected, the AI alerts the relevant teams, allowing them to shift subsequent cases or notify the next surgical team well in advance. This proactive approach has significantly reduced the frantic, reactive communication that typically characterizes a busy surgical day. By providing a continuous stream of accurate data, the platform ensures that every stakeholder, from the anesthesia team to the sterile processing department, is working from the same set of real-time facts.
Fostering Transparency Through People-Centric Strategies
The successful adoption of AI at MUSC Health was not merely a technological feat but also a triumph of organizational strategy and stakeholder engagement. Recognizing that new technology can often be perceived as an intrusive monitoring tool, the health system established a governance committee led by surgeon champions to oversee the rollout. These leaders were instrumental in defining the ethical guardrails and operational goals of the project, ensuring that the AI was marketed as a clinical support tool rather than a punitive oversight mechanism. By involving physicians early in the process and allowing them to help shape the metrics being tracked, the institution fostered an environment of transparency and mutual respect that facilitated a smooth transition across departments.
As the platform became an integral part of the daily routine, its utility led to organic growth in adoption that far exceeded the initial scope of the project. While the system was originally intended for perioperative leadership, demand quickly spread to pre-operative and post-operative units, as well as anesthesia teams who saw the value in having a real-time pulse on the surgical floor. This expanded access has unified the various components of the surgical care continuum, allowing for better coordination between teams that were previously siloed. The shift in perspective was profound; rather than viewing the AI as a “big brother” figure, staff began to see it as an essential partner that reduced their administrative workload and provided them with the information needed to perform their jobs more effectively and with less stress.
Leveraging Data to Transform Surgical Performance
Debunking Assumptions with High-Fidelity Analytics
One of the most immediate benefits of the AI-driven data was its ability to challenge and debunk long-standing institutional myths regarding surgical delays. For years, the prevailing belief among staff was that slow room turnovers were primarily the result of inefficient environmental services or cleaning protocols. However, a deep dive into the high-fidelity data revealed a much more complex reality. The AI showed that the actual cleaning time was often well within acceptable limits, but significant “idle time” was occurring after the room was clean and before the next patient arrived or the setup began. This insight proved that the bottleneck was not a sanitation issue but a coordination and communication gap between different teams.
Furthermore, the data highlighted a stark contrast between the accuracy of manual logs and the AI-generated timestamps. Analysis showed that the AI-captured events were six times more accurate than the corresponding entries in the electronic health record, which were often delayed by up to 45 minutes. This level of precision allowed management to perform a granular “anatomy of a turnover,” breaking down every minute spent between cases to identify specific opportunities for improvement. By shifting the focus from broad generalizations to specific, actionable data points, MUSC Health was able to implement targeted interventions that addressed the actual root causes of inefficiency. This evidence-based approach has not only improved throughput but also validated the efforts of the staff by correctly identifying where the real challenges lay.
Maximizing Capacity Through Accurate Scheduling
Beyond improving daily turnovers, the AI platform has provided invaluable insights into the broader patterns of surgical scheduling and capacity management. The analytics revealed significant discrepancies in how cases were being booked, with approximately 28% of procedures being underscheduled by more than half an hour. These errors frequently led to a domino effect of delays, forcing staff to work unplanned overtime and creating a high-stress environment for both providers and patients. Conversely, 20% of cases were overscheduled, creating pockets of “white space” that represented wasted capacity. By identifying these patterns, MUSC Health has been able to refine its scheduling algorithms to better match the actual time required for specific surgeons and procedures.
This newfound ability to redistribute surgical volume more effectively has allowed the institution to maximize the utility of its existing footprint without the need for costly physical expansions. By filling the gaps created by overscheduling and providing more realistic buffers for complex cases, the health system has improved its overall throughput while simultaneously reducing the burnout associated with unpredictable workdays. The precision of the data allows for a more equitable distribution of the surgical workload, ensuring that every operating room is utilized to its highest potential. This shift toward predictive, data-driven scheduling ensures that the institution can accommodate more patients while maintaining a stable and sustainable environment for its clinical staff.
Enhancing the Future of Perioperative Management
The transition to a proactive operational model at MUSC Health has set a new benchmark for how ambient artificial intelligence can be leveraged to solve chronic problems in healthcare management. By moving away from reactive decision-making based on untrusted or incomplete data, the institution has created a more resilient and efficient surgical ecosystem. The lessons learned from this implementation suggest that the future of hospital operations lies in the seamless integration of machine precision with human clinical expertise. This approach does not replace the judgment of medical professionals but rather empowers them with the high-fidelity information they need to make the best possible decisions for their patients and their teams.
As healthcare continues to evolve, the ability to turn time—a hospital’s most constrained and valuable resource—into a manageable asset will be a key differentiator for leading institutions. The success at MUSC Health serves as a blueprint for other organizations looking to optimize their perioperative suites through the use of “ground-truth” data and predictive analytics. Looking ahead, the integration of these tools will likely expand into other areas of the hospital, creating a fully connected and data-driven care environment. By embracing these technological advancements today, healthcare leaders can ensure they are prepared to meet the demands of tomorrow, maintaining the highest standards of surgical care in an increasingly complex and resource-constrained landscape. Past practices of manual tracking are being phased out in favor of this transparent, automated future.