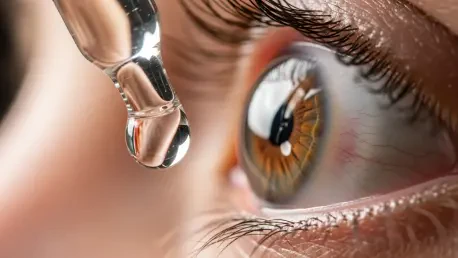
When a routine visit to the local pharmacy results in the purchase of a common healthcare staple, few consumers anticipate that their trusted lubricating eye drops might harbor invisible risks due to manufacturing failures. The recent announcement by the Food and Drug Administration regarding the recall of over three million units of ophthalmic products highlights a significant breakdown in the specialized protocols required for sterile medical production. This massive recall, initiated by California-based manufacturer K.C. Pharmaceuticals, encompasses dozens of popular store brands that millions of Americans rely on for daily relief from dryness and irritation. While current reports have not confirmed active bacterial contamination in every bottle, the fundamental inability of the producer to guarantee sterility has triggered an immediate and widespread removal of these items from retail shelves across the entire country to prevent potential injuries. This situation underscores the delicate nature of the global medical supply chain where a single facility serves numerous competitors.
Implications of Manufacturing Deficiencies
Sterility Concerns: Assessing the Risk Factors
The primary concern cited by the regulatory authorities involves a critical lack of assurance regarding the sterility of the manufacturing environment, which is a non-negotiable requirement for any product applied to the eye. Ophthalmic solutions must be entirely free of microbial life because the ocular surface is highly vulnerable to infection, and introducing unsterile liquid can bypass the body’s natural defenses. Even though the manufacturer has not identified a specific pathogen currently present in the distributed lots, the admission that sterile standards could not be verified means the entire production run is effectively compromised from a safety standpoint. This technical failure creates a window of opportunity for harmful bacteria or fungi to proliferate within the bottles, potentially leading to severe conditions such as keratitis or permanent vision loss. Consequently, the medical community remains on high alert as they monitor for any reports of adverse reactions linked to these specific batches.
This massive safety intervention covers a diverse array of products, ranging from standard artificial tears to specialized redness lubricants and ultra-lubricating formulas designed for chronic dry eye relief. The technical nature of the recall is further complicated by the sheer volume of material, with over 3.1 million bottles currently circulating in the marketplace or sitting in consumer medicine cabinets. Investigators have pointed to specific lot number prefixes including AC, AR, LT, SU, RG, RL, SY, and AT as the primary markers for identification. Because many of these products were manufactured with long-term stability in mind, their expiration dates extend well into 2026, creating a persistent risk if consumers do not actively check their current inventory. The breadth of the affected product types suggests that the sterility issues were not isolated to a single machine or production line but were instead systemic within the facility during the specific manufacturing period.
Distribution Networks: The Reach of Store Brands
The geographical and commercial scope of this recall is exceptionally broad, illustrating how a single manufacturing point can impact a vast segment of the retail landscape through private-label agreements. National pharmacy giants such as CVS Health, Walgreens, and Rite Aid are all featured prominently on the recall list, alongside major grocery chains like Kroger, Publix, and H-E-B. This phenomenon occurs because many retailers do not manufacture their own generic medications; instead, they contract with third-party producers like K.C. Pharmaceuticals to provide products that meet specific price points and formulations. When a failure occurs at this central node, the resulting recall ripples through discount stores like Dollar General and even industrial suppliers like Cintas. This interconnectedness means that a consumer in a rural area buying a discount brand faces the exact same manufacturing risks as a shopper in a major city purchasing a premium pharmacy-labeled product.
Beyond the retail storefront, the distribution network includes wholesale giants like Cardinal Health and McKesson, which provide supplies to hospitals, clinics, and independent pharmacies. This deep penetration into the healthcare infrastructure signifies that the recalled eye drops could be found in professional medical settings just as easily as in a home bathroom. The logistical challenge of retrieving over three million bottles is unprecedented, requiring a coordinated effort between the manufacturer, federal regulators, and thousands of individual retail locations. This event serves as a stark reminder of the hidden complexities within the pharmaceutical industry, where brand names often mask a shared production origin. As the recall progresses, the emphasis remains on transparency, ensuring that every entity in the supply chain communicates the risks effectively to the end-user, regardless of whether the product was purchased at a luxury grocer or a neighborhood convenience store.
Navigating the Recovery and Safety Protocols
Identification Procedures: Verifying Product Integrity
For consumers who currently use over-the-counter eye care products, the immediate priority is a manual inspection of all containers to verify their safety status against the FDA-published list. The critical information is typically located on the bottom of the box or the side of the plastic bottle, where the lot number and expiration date are stamped. If a bottle features the prefixes identified in the recall, such as LT or SY, it should be isolated and removed from use immediately to prevent accidental application. Health experts emphasize that even if a bottle appears clear and the liquid does not look cloudy, the absence of sterility cannot be detected by the naked eye. Using a potentially contaminated product poses a gamble with ocular health that outweighs any temporary relief provided by the drops. If the packaging has already been discarded, making it impossible to verify the lot number, the safest course of action is to err on the side of caution and dispose of the remaining product.
Once a recalled item has been identified, the next step involves navigating the return and refund process, which varies significantly depending on the retailer where the purchase was made. While the manufacturer handles the overarching logistics of the recall, individual stores like Walgreens or CVS often have their own protocols for handling customer returns of defective medical goods. Most major retailers are expected to offer full refunds or exchanges for safe alternatives, even if the consumer no longer possesses the original receipt, provided the product clearly belongs to the affected lot. In addition to securing a refund, patients who have been using these drops should consult with an eye care professional, especially if they have noticed any redness, discharge, or unusual pain. Pharmacists are also valuable resources during this time, as they can recommend alternative brands that were not produced at the K.C. Pharmaceuticals facility and remain safe for use throughout the remainder of the year.
Future Safeguards: Strengthening Ophthalmic Oversight
The resolution of this massive recall necessitated a comprehensive re-evaluation of how generic ophthalmic products are monitored and verified before they reach the consumer. Moving forward through 2026 and into 2027, the industry began implementing more rigorous real-time sterility testing protocols that offer faster detection of environmental failures within cleanroom settings. Regulatory bodies also increased the frequency of unannounced inspections for third-party manufacturers who supply multiple retail labels, recognizing that a single point of failure now carries a much higher systemic risk than in previous decades. This shift toward proactive surveillance was designed to identify potential issues with airflow, water purification, and equipment sterilization before products are bottled and shipped. For the consumer, these changes resulted in more transparent labeling, often including digital QR codes that allowed for instant verification of a product’s safety status and manufacturing history via a smartphone.
The industry successfully transitioned toward a more resilient supply chain model that prioritized safety over the speed of production. Manufacturers adopted advanced robotic filling systems that minimized human contact with sterile solutions, further reducing the possibility of accidental microbial introduction. Retailers, in turn, established more direct oversight of their private-label partners, requiring independent audits and higher standards of quality assurance as a prerequisite for contract renewal. This collaborative approach ensured that the lessons learned from the K.C. Pharmaceuticals incident were codified into new standard operating procedures for the entire pharmaceutical sector. By the time the industry looked toward 2028, the protocols for managing store-brand medical supplies had become significantly more robust, providing consumers with renewed confidence that the affordable healthcare products they purchased were manufactured with the highest possible commitment to safety and clinical excellence.