In an environment where diagnostic speed often dictates the outcome of critical medical emergencies, the pervasive use of advanced imaging technology has reached unprecedented levels across the modern healthcare landscape. Recent data reveals that in 2023 alone, the United States healthcare system facilitated over 93 million scans distributed among 62 million individual patients, representing a massive technological reliance that has sparked significant debate. A landmark study published in JAMA Internal Medicine during February 2026 indicates that this volume of ionizing radiation exposure might lead to approximately 103,000 additional cancer cases over the lifetimes of those scanned. This figure accounts for nearly five percent of all new annual cancer diagnoses, suggesting that the very tools used to save lives may carry a delayed biological cost. While these procedures provide immediate clarity for physicians, the sheer scale of exposure requires a reevaluation of how medical professionals balance urgent diagnostic needs against the potential for secondary health complications decades later.
Identifying the Most Vulnerable Patient Demographics
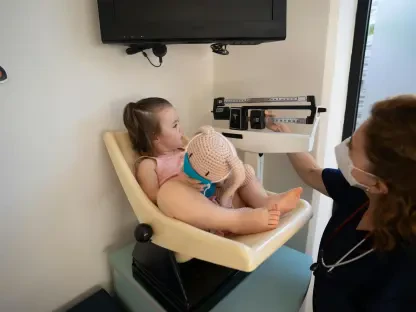
The susceptibility to radiation-induced cellular damage is not uniform across the human population, as physiological factors such as age and developmental stage play a decisive role in determining long-term risk. Pediatric patients, particularly infants under the age of one, remain the most vulnerable demographic due to the rapid rate of cell division occurring within their developing tissues and organs. Because children have a much longer life expectancy ahead of them, any genetic mutations triggered by ionizing radiation have more time to manifest into clinical malignancies. Experts note that a single CT scan administered in infancy carries a higher statistical weight for future complications than the same procedure performed on an elderly adult. Consequently, the medical community has begun prioritizing specialized pediatric protocols that adjust radiation dosages to the smallest possible levels. This demographic sensitivity underscores the necessity of tailoring imaging strategies to the individual patient rather than applying a standardized approach that ignores the unique biological vulnerability of younger populations.
Biological sex also influences how the body reacts to the invisible energy of diagnostic beams, with women showing a disproportionately higher susceptibility to specific types of cancer following exposure. Research suggests that even when receiving identical radiation doses, female patients are more likely to develop thyroid and breast cancers compared to their male counterparts. This discrepancy stems from the radiosensitivity of glandular tissues, which can be inadvertently affected during scans of the chest or neck areas. Furthermore, the risk for most adults is rarely tied to a single, isolated examination but rather to the cumulative radiation dose accumulated over years of repeated diagnostic procedures. As patients navigate chronic conditions that require frequent monitoring, the total volume of exposure builds up, potentially crossing a threshold where the body’s natural repair mechanisms are overwhelmed. Recognizing these specific biological variances allows healthcare providers to implement more precise safety measures, ensuring that the most sensitive organs are shielded whenever possible during high-resolution imaging sessions.
Innovations in Diagnostic Safety and Accuracy
In response to growing concerns regarding cumulative exposure, the medical technology sector has accelerated the development of sophisticated tools designed to minimize radiation without sacrificing image quality. Modern facilities are increasingly adopting low-dose imaging protocols and iterative reconstruction algorithms that allow for high-clarity visuals with a fraction of the energy traditionally required. Furthermore, the integration of artificial intelligence into the clinical workflow is proving to be a game-changer for radiation safety. Advanced AI systems, such as those implemented in GE HealthCare’s TrueFidelity or Siemens Healthineers’ AI-Rad Companion, assist radiologists in optimizing dose parameters for each specific patient. These platforms can analyze a patient’s body habitus and previous scan history to suggest the most efficient settings, ensuring that no excess radiation is utilized. By utilizing these intelligent systems, hospitals can maintain the diagnostic power of computed tomography while significantly lowering the statistical probability of inducing long-term cellular damage in patients who require frequent imaging.
The paradigm shift toward responsible imaging also involves a rigorous assessment of whether ionizing radiation is the only viable path for a specific diagnosis or if safer alternatives exist. In many clinical scenarios, non-ionizing modalities such as magnetic resonance imaging or specialized ultrasound techniques can provide sufficient data to guide treatment plans. This approach is particularly relevant for abdominal and pelvic imaging, which currently contribute to more than 37,000 projected future cancer cases due to the high dosages often required for these complex regions. Medical societies now encourage a “triple-question” framework for both providers and patients: Is the scan truly necessary for the immediate diagnosis? Are there alternative methods available that do not involve radiation? How exactly will the results of this scan alter the current treatment strategy? By addressing these questions before ordering a procedure, clinicians can avoid redundant testing and focus on the most effective, least invasive diagnostic pathways. This cultural change in medicine prioritizes long-term patient wellness alongside immediate clinical intervention needs.
Future Pathways for Integrated Patient Care
The medical community successfully established comprehensive tracking systems to record lifetime radiation exposure for every patient, treating it with the same level of scrutiny as a prescription drug history. This evolution in data management allowed physicians to make more informed decisions by weighing the immediate benefits of a new scan against the total cumulative dose already recorded in a patient’s electronic health record. Educational initiatives empowered patients to take an active role in their diagnostic journey, fostering a transparent dialogue about the risks and benefits associated with various imaging technologies. Researchers also focused on developing biological markers that could predict an individual’s personal sensitivity to radiation, moving away from generalized statistics toward truly personalized medicine. These advancements ensured that the life-saving potential of medical scans was maximized while the long-term risks remained meticulously managed. Ultimately, the industry transitioned from a reactive stance on radiation safety to a proactive model that integrated technological innovation with a deep commitment to patient safety and long-term health outcomes.