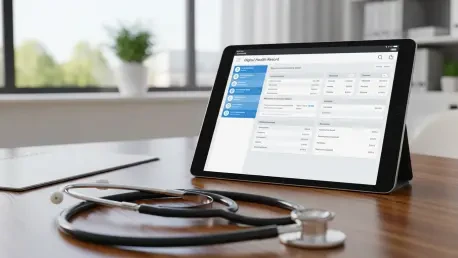
The persistent reliance on legacy fax machines in a high-tech era has long been a bottleneck for healthcare efficiency, leading to fragmented patient data and delayed treatments across the province. On May 9, 2026, Quebec took a decisive step to rectify this by launching its new Digital Health Record (DSN) at two primary showcase locations. These sites, CIUSSS du Nord-de-l’Île-de-Montréal and CIUSSS de la Mauricie-et-du-Centre-du-Québec, serve as the testing grounds for a system designed to consolidate over four hundred disparate computer platforms into a single interoperable network. This modernization replaces paper forms with real-time alerts and streamlined data sharing, aiming to eliminate the redundancies that frequently plague clinical workflows. By centralizing information, the platform intends to enhance patient safety and provide healthcare providers with a clearer, more holistic view of a patient’s medical history during critical decision-making moments. This transition represents a fundamental shift in how the province manages its medical infrastructure, moving away from siloed archives toward a unified digital ecosystem.
Navigating the Challenges: Technological and Financial Implementation
Transitioning to such a massive digital infrastructure is rarely a seamless process, and Health Minister Sonia Bélanger has already cautioned that the coming weeks will likely involve technical glitches and a steep learning curve for hospital staff. To mitigate the inevitable friction of this shift, Santé Québec has deployed 3,200 specialized “superusers” to offer on-site support and troubleshoot issues as they arise in real-time. This hands-on approach is essential because the complexity of migrating clinical data from antiquated databases into a modern interface can often lead to temporary disruptions in patient intake and administrative processing. While the government remains optimistic about the long-term benefits, healthcare workers and opposition parties have expressed concerns regarding the stability of the software and the potential for security breaches. Ensuring that these frontline workers are adequately trained remains a top priority to prevent burnout and ensure that the digital transition does not inadvertently compromise the quality of bedside care during this initial rollout phase.
Beyond the clinical implications, the financial scope of the DSN project reflects the scale of the commitment to healthcare modernization, with the initial pilot alone requiring an investment of four hundred million dollars. The projected cost for a full province-wide expansion ranges between one and a half billion to three billion dollars, a figure that has sparked intense debate regarding fiscal responsibility. However, administrative officials argued that the long-term economic benefits outweighed the steep initial price tag. Although the system carried an estimated annual operating cost of one hundred million dollars, it was expected to generate approximately one hundred and twenty million dollars in yearly savings through increased operational efficiency and the reduction of unnecessary diagnostic tests. This financial strategy relied on the ability of the system to provide managers with real-time data to monitor performance and optimize resource allocation across the network. By shifting from reactive management to a data-driven model, the government hoped to create a sustainable healthcare ecosystem that could withstand the pressures of an aging population.