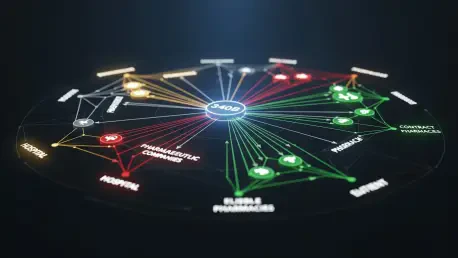
The transformation of the 340B drug pricing program from a targeted federal safety net into a massive, multi-billion-dollar profit center has ignited a fierce legislative debate within the halls of Congress. Originally established to assist healthcare providers in stretching scarce federal resources to reach more eligible patients, the program has grown into a $65 billion revenue stream that lacks robust federal oversight or clear mandates for patient benefit. Current data reveals a troubling trend where tax-exempt hospitals and their for-profit partners leverage the steep discounts intended for the vulnerable to pad their bottom lines instead of lowering out-of-pocket costs for individuals. This shift has created an environment where the original mission of the program is frequently overshadowed by aggressive financial strategies designed to maximize the spread between discounted acquisition costs and full-market reimbursements. As a result, the very populations the program was meant to protect often find themselves still struggling with high medication costs while the institutions serving them reap record-setting financial rewards from the pricing gap.
The Economic Divide: Examining Market Distortions and Revenue Growth
Under the current regulatory framework, eligible facilities can purchase prescription medications at extremely low prices, sometimes paying as little as one penny for high-cost treatments. However, these institutions frequently charge patients and private insurers the full market price, pocketing the massive difference as pure profit. A recent investigation into the healthcare landscape in Minnesota highlighted the sheer scale of this practice, showing that hospitals and their various for-profit intermediaries generated approximately $1.34 billion in profit from the program in just one year. This markup practice is not an isolated incident but rather a systemic feature that has incentivized hospitals to expand their 340B footprints into affluent suburbs rather than focusing on the underserved urban or rural areas where the need is greatest. The absence of strict reporting requirements means that there is no clear way to verify if these substantial profits are reinvested into charity care or if they are simply being used to subsidize general operating expenses or executive compensation packages.
There is a growing bipartisan consensus in Washington that the program requires an urgent overhaul to prevent further exploitation by large healthcare systems. Both the Senate Health, Education, Labor and Pensions Committee and the House Energy and Commerce Committee have initiated comprehensive hearings to investigate the rapid expansion of the program and its impact on the wider pharmaceutical market. Legislators have correctly identified a critical flaw in the existing law: it contains no guardrails or specific legal requirements that mandate hospitals must pass their 340B savings directly to the low-income patients they serve. This policy vacuum has allowed the program to balloon in size without a corresponding increase in the level of charity care provided by participating institutions. Moreover, the lack of transparency complicates efforts by federal regulators to track the flow of money, making it nearly impossible to ensure that the billions of dollars circulating through the system are achieving the intended public health outcomes or if they are merely inflating the cost of care for everyone else.
Strategic Imperatives: Implementing Solutions for Long-Term Sustainability
Lawmakers recognized that maintaining the status quo was no longer an option if they intended to preserve the integrity of the nation’s healthcare safety net. To address these systemic failures, federal authorities prioritized the implementation of common-sense accountability measures that required hospitals to provide detailed disclosures regarding their 340B revenue and its specific application toward patient discounts. This transition moved away from vague promises of community benefit and toward a standardized reporting system that ensured transparency at every level of the supply chain. Policymakers also explored the creation of mandatory pass-through requirements, which ensured that a significant portion of the discount reached the patient at the pharmacy counter. By refocusing the program on direct affordability rather than institutional revenue, the reform efforts sought to lower the overall financial burden on the healthcare system. These legislative actions provided a clearer roadmap for future drug pricing policies, emphasizing that any federal discount program must be paired with rigorous oversight to remain effective and sustainable.