Taiwan’s current healthcare landscape is undergoing a radical transformation as medical technologists emerge from the background to occupy a central role in the nation’s survival strategy. During the recent 17th Asia-Pacific Forum of Medical Laboratory Science held in Taichung, the focus shifted toward viewing these professionals not just as laboratory staff, but as the primary eyes of the medical system. Their ability to provide early disease detection, complex clinical diagnostics, and continuous post-treatment monitoring forms the foundation upon which all modern medical decisions are built. The government has identified these specialists as crucial pillars in precision medicine and public health resilience, especially as systemic pressures from a rapidly aging population mount. By reinforcing the diagnostic infrastructure, the state aims to ensure that every clinical decision is backed by high-fidelity data, thereby reducing the margin for error in patient care. This evolution represents a strategic shift where laboratory science is no longer a secondary service but a lead driver of national health security.
The Technological Shift Toward Smart Diagnostic Protocols
The integration of artificial intelligence and automated testing represents the next phase of development for Taiwan’s medical facilities, ensuring that laboratories remain sustainable despite rising caseloads. Smart laboratory protocols are now being designed to handle the heavy lifting of routine analysis, allowing human experts to focus on the interpretation of complex genomic data and rare pathological markers. By 2026, the transition toward these automated systems has already begun to yield significant improvements in diagnostic precision, enabling medical professionals to identify potential health risks long before symptoms manifest. This surge in technical capability is central to the broader Healthy Taiwan initiative, which seeks to modernize every facet of the diagnostic pipeline. The goal is to create a seamless flow of information from the test tube to the electronic health record, reducing human error and accelerating the delivery of life-saving results. As these technologies become more deeply embedded in the clinical workflow, they provide the necessary scalability to meet the demands of a modern, data-driven healthcare environment.
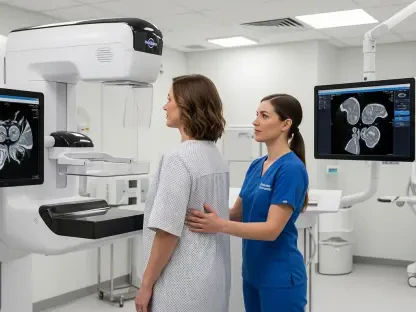
Precision medicine relies heavily on the ability of laboratory technologists to harness cutting-edge digital tools that provide a granular view of a patient’s unique biological landscape. These professionals are increasingly utilizing high-throughput sequencing and advanced biosensors to monitor everything from viral loads to the efficacy of personalized cancer therapies in real-time. This level of detail is essential for the proactive management of chronic diseases, which currently place a significant strain on national resources. Moreover, the resilience of the healthcare infrastructure is being fortified through the adoption of decentralized testing and point-of-care diagnostics, which ensure that high-quality medical analysis is available even in remote or underserved areas. By leveraging the country’s existing strengths in the semiconductor and information technology sectors, the biomedical industry is creating a robust ecosystem where hardware and biology converge. This synergy not only enhances the quality of local patient care but also establishes a global benchmark for how advanced technology can be successfully applied to public health challenges on a national scale.
Navigating the Challenges of a Super-Aged Society
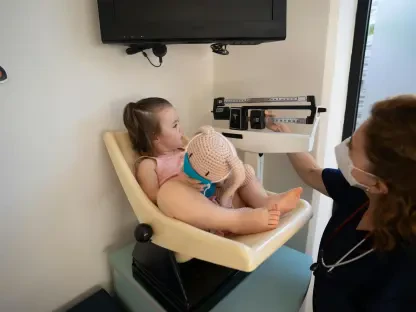
Taiwan’s shift toward a super-aged demographic necessitates a fundamental move from reactive treatment models to a comprehensive system of health promotion and disease prevention. The traditional approach of waiting for an illness to reach a critical stage before intervening is no longer sustainable under the weight of rising healthcare costs and a shrinking workforce. Instead, the focus has pivoted toward using laboratory science as an early warning system that detects metabolic shifts or early-stage cancers during routine screenings. This proactive stance is the core of the government’s long-term strategy to maintain national productivity and ensure a high quality of life for the elderly. By implementing mass screening programs powered by smart diagnostic tools, the health system can manage the health of the entire population more efficiently. These efforts are complemented by a renewed emphasis on public health education, where laboratory data is used to inform individuals about their specific health risks. The result is a more informed citizenry that actively participates in its own wellness, significantly reducing the frequency of emergency medical interventions and long-term hospital stays.
Addressing the systemic impacts of climate change and extreme weather events also requires a resilient medical laboratory network that can respond to emerging infectious diseases with speed and accuracy. The ability to pivot laboratory resources toward infection control and environmental health monitoring is vital for maintaining social stability during unpredictable crises. As the prevalence of chronic conditions rises, the demand for sophisticated monitoring and risk assessment services will only continue to grow, placing laboratory science at the forefront of the national security agenda. The administration has committed to expanding investment in the biomedical sector to ensure that high-tech innovations are rapidly integrated into clinical practice. This involves not only the procurement of advanced machinery but also the continuous professional development of technologists who must navigate an increasingly complex digital landscape. By fostering a culture of innovation, the state ensures that its healthcare system remains flexible and capable of adapting to the evolving needs of its people. This commitment to progress is what defines the intersection of technology and industry, creating a path toward a sustainable future where health and economic growth are inextricably linked.
Building Resilience Through International Collaboration
Strengthening global partnerships through platforms such as the Asia-Pacific Forum of Medical Laboratory Science has proven essential for sharing best practices and standardizing diagnostic protocols across borders. These international exchanges allowed for the rapid dissemination of new methodologies in smart laboratory management and helped to harmonize the regional response to public health threats. By collaborating with experts from diverse backgrounds, local technologists gained access to a wider pool of knowledge, which in turn elevated the quality of medical services provided domestically. This spirit of cooperation fostered a robust network of professionals who were committed to advancing the field of medical science through collective effort. Such partnerships also opened new avenues for industrial growth, as domestic biomedical firms found opportunities to export their innovations to broader markets within the Asia-Pacific region. The synthesis of professional expertise and digital tools served as the definitive path toward a sustainable medical system, ensuring long-term public health and regional stability. This collaborative approach ensured that no single nation had to face the complexities of modern medicine in isolation, reinforcing the collective resilience of the entire global healthcare community.
Future considerations for the medical laboratory sector focused on the continuous refinement of data privacy frameworks and the ethical implementation of artificial intelligence in clinical settings. The development of clear guidelines for the use of patient data was identified as a critical step in maintaining public trust while still allowing for the breakthroughs promised by machine learning. It was determined that the most effective way forward involved creating a standardized digital infrastructure that supported interoperability between different healthcare providers and international partners. Actionable steps were taken to incentivize the adoption of sustainable laboratory practices, reducing the environmental footprint of medical testing without compromising on diagnostic accuracy. Investment in specialized training programs ensured that the next generation of medical technologists possessed the skills required to lead in a technology-driven environment. By prioritizing the human element alongside technological advancement, the healthcare sector established a balanced model that prioritized both efficiency and empathy. These initiatives collectively moved the nation toward a more resilient and integrated medical ecosystem, securing a healthier future through the strategic application of laboratory science and international solidarity.