Understanding the Judicial Shield Around Arbitration Awards
The escalating financial stakes in the multi-billion dollar healthcare reimbursement market have reached a boiling point as federal courts begin to cement the finality of independent arbitration awards. This development marks a significant transition from open litigation to a closed administrative ecosystem, forcing insurance giants to reconsider their long-term legal strategies. While the No Surprises Act was originally designed to protect patients from financial ruin, it has inadvertently sparked a corporate war over payment rates and billing practices. As judges dismiss high-profile lawsuits, the industry is left wondering if the Independent Dispute Resolution process has become an untouchable mechanism of federal law.
Recent judicial trends suggest that the door to the courthouse is closing for those seeking to overturn unfavorable arbitration outcomes. Insurers have attempted to argue that systemic fraud and manipulation of the system should allow for federal intervention, yet the courts remained steadfast in their support of the administrative framework. This shift has profound implications for how capital is allocated within the healthcare sector, as the certainty of arbitration awards becomes a cornerstone of financial planning for both large-scale provider groups and national insurance carriers.
The Legislative Foundation: How the No Surprises Act Changed Billing
Before the landmark implementation of the No Surprises Act, the healthcare sector operated under a system of private negotiation that frequently left patients vulnerable to exorbitant out-of-network costs. This legislative shift redirected the conflict away from consumers and into a structured arbitration framework where third-party mediators decide payment amounts. This transition was intended to simplify billing, yet it created a new arena for strategic financial maneuvering. By establishing the Independent Dispute Resolution process, the federal government fundamentally changed how value is determined in medical services, effectively ending the era of unilateral billing power.
The movement toward this centralized system has not been without its critics, who argue that the complexity of the law creates new inefficiencies. Since the act took effect, the volume of disputed claims has far exceeded initial government estimates, leading to a massive backlog that has tested the resilience of the arbitration system. This high-pressure environment has forced both insurers and providers to adopt more aggressive postures, leading to the current wave of litigation as parties seek to test the boundaries of the law’s administrative authority.
Analyzing the Legal Battle Between Insurers and Large Provider Groups
Allegations of Systemic Manipulation and Fraudulent Billing
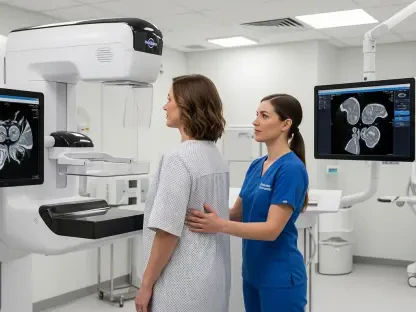
The recent legal friction is best seen through the lens of major lawsuits against large-scale radiology groups. Insurers alleged that certain providers engaged in systemic manipulation by funneling claims through specific entities that lacked in-network contracts. This tactic supposedly forced disputes into the arbitration system, where mediators often grant awards that far exceed historical market rates. Carriers argued that this behavior constituted a fraudulent attempt to bypass negotiated agreements, turning a patient protection law into a profit-maximizing tool for medical conglomerates.
Furthermore, the scale of these operations suggests a highly coordinated effort to leverage the nuances of federal law. By treating services performed by in-network doctors as out-of-network claims through clever billing structures, providers were accused of “gaming” the system for billions in additional revenue. This alleged exploitation of the law’s loopholes has become a primary point of contention for insurers who believe the arbitration process is being used as a weapon rather than a shield for fair compensation.
The Growing Judicial Consensus Against Post-Arbitration Litigation
Despite the severity of these allegations, the judicial response has been overwhelmingly consistent in favor of administrative finality. Recent rulings indicate that the federal court system is not an appropriate venue for secondary appeals of arbitration decisions. Judges emphasized that any grievances regarding billing eligibility or fraudulent claims must be addressed during the mediation phase itself. This trend toward judicial restraint suggests that insurers can no longer rely on federal courts to unwind unfavorable financial outcomes once the process has concluded.
This legal stance reinforces the idea that the No Surprises Act is a self-contained system. By refusing to hear these cases, the courts are essentially directing all future disputes back into the hands of government-certified arbiters. This creates a significant hurdle for insurers, as they must now prove their case within a much tighter timeframe and under the specific rules of the arbitration framework, rather than through the broader discovery processes available in federal litigation.
Navigating the Financial and Administrative Complexities of the IDR Process
The financial magnitude of this shift is staggering, with a handful of large provider organizations accounting for nearly half of all resolved claims in the past few years. These disputes involve billions of dollars and represent a significant administrative burden that contributes to rising system costs. While providers argued that the system ensured fair pay in a market dominated by massive insurance carriers, the result was a bottleneck of claims that strained federal resources. This tension highlights the growing divide between the administrative reality of healthcare billing and the strategic goals of the participants.
Moreover, the administrative costs of managing these disputes have become a significant line item for both parties. The need for specialized legal and billing teams to navigate the arbitration process has added layers of bureaucracy to an already complex system. As the volume of claims continues to grow, the pressure on the federal government to streamline these processes increases, leading to potential shifts in how arbiters are selected and how their decisions are rendered in the future.
Future Implications for Healthcare Regulation and Litigation
Looking toward the future, the lack of judicial intervention will likely prompt federal agencies to refine the regulatory rules governing the arbitration process. We can anticipate more stringent oversight from the Department of Health and Human Services to prevent the perceived “gaming” of the system. This could include new reporting requirements for provider groups and more rigorous audits of billing subsidiaries. As the government seeks to maintain the integrity of the act, the focus will shift from the courtroom to the regulatory drafting table.
Furthermore, as litigation remains a dead end, insurers will likely pivot toward advanced technological solutions for front-end fraud detection and eligibility verification. This evolution suggests that the next phase of the No Surprises Act will be defined by technical compliance and rigorous pre-arbitration scrutiny. The winners in this new landscape will be those who can most effectively use data and automation to identify and challenge problematic claims before they ever reach the arbitration stage.
Strategic Recommendations for Navigating the NSA Landscape
For market participants, the recent legal developments demanded a fundamental shift in how billing disputes were managed. Insurers needed to prioritize internal audits and ensure that all technical objections were fully documented before a claim ever reached the arbitration table. Relying on post-award litigation proved to be an ineffective and costly strategy that failed to yield results. Proactive engagement during the initial negotiation periods was the only way to mitigate the risk of inflated awards.
At the same time, providers were required to align their corporate structures with federal transparency standards to withstand the increasing pressure from carrier-led investigations. Transparency became the primary defense against accusations of systemic manipulation. Both parties found that investing in clearer communication channels helped to resolve many disagreements before they escalated into the federal arbitration system, thereby reducing the high overhead associated with the independent dispute resolution process.
The Final Verdict: Why the IDR Process Remains Supreme
The dismissal of major lawsuits confirmed that the Independent Dispute Resolution process remained the supreme authority in healthcare reimbursement. By upholding the finality of these awards, the judiciary reinforced the self-contained nature of the No Surprises Act ecosystem. Insurers found that their recourse was limited to administrative advocacy rather than the federal witness stand. The courts effectively shielded the arbitration process from external legal challenges, ensuring that the system functioned as the ultimate arbiter of medical value.
Ultimately, the industry learned that the strength of a billing claim was determined at the arbitration table, where the rules of federal law reigned absolute and unchallenged by traditional litigation. The transition toward this administrative model signaled a permanent change in the power dynamics of the healthcare market. As the sector moved forward, the focus remained on mastering the technicalities of the law rather than hoping for a judicial rescue from the financial consequences of unfavorable arbitration outcomes.