The global medical community currently stands at a transformative crossroads where the successful development of radioligand therapies faces the stark reality of a strained and aging production infrastructure. As of 2026, the Third International Workshop on Medical Radioisotope Supply has emphasized that while the scientific foundation for these life-saving treatments is robust, the physical supply chain remains a precarious bottleneck for patients worldwide. Over 130 experts from clinical medicine, government policy, and nuclear research recently convened to address this disparity, highlighting that the era of speculative research has officially transitioned into a demand-driven industrial challenge. The primary focus of modern nuclear medicine is no longer just the discovery of new isotopes but the creation of a reliable, high-volume delivery system. Without a coordinated global effort to scale production, the breakthrough treatments currently offering hope to cancer patients may remain out of reach for the majority of the population who need them most.
Reshaping the Global Isotope Market
Diversification of Production: A Technical Shift
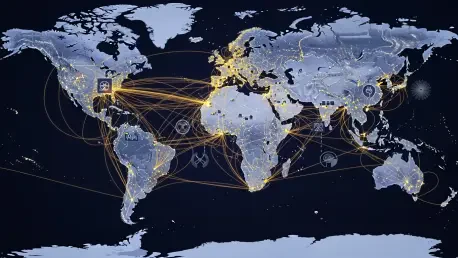
The historical reliance on a few aging nuclear reactors for the production of Molybdenum-99, the precursor to the most widely used diagnostic isotope, has created a legacy of vulnerability that the industry is now aggressively moving to correct. There is a decisive shift toward a more diverse isotopic portfolio, prioritizing therapeutic agents such as Lutetium-177 and Actinium-225 which are essential for the latest generation of targeted oncology treatments. By diversifying the isotope menu, the medical community aims to provide precision tools for a wider array of cancers, but this requires a fundamental change in how these materials are manufactured. The transition from a centralized model to a decentralized network is intended to mitigate the risk of regional outages that have historically paralyzed nuclear medicine departments. This shift ensures that if one facility faces maintenance or regulatory downtime, other nodes within the global network can absorb the demand without compromising patient care or treatment timelines.
Building this resilience necessitates the simultaneous utilization of both traditional high-flux nuclear reactors and modern particle accelerator technologies. While reactors remain the workhorse for producing large quantities of certain isotopes, linear accelerators and cyclotrons offer a cleaner, more targeted approach for generating alpha-emitters like Actinium-225. This dual-track strategy is critical because it reduces the dependence on any single technology or geographic location, creating a redundant and stable supply environment. Furthermore, the integration of accelerator-based production allows for the manufacturing of isotopes with higher specific activity, which is vital for the effectiveness of radioligand therapies. As facilities are upgraded or newly constructed, the focus is on creating a modular infrastructure that can quickly adapt to the changing needs of the pharmaceutical industry. This technical agility is the cornerstone of a secure supply chain that can keep pace with the rapid advancements occurring in the clinical trials of new radio-pharmaceuticals.
Private Capital and Vertical Integration: New Business Models
The landscape of radioisotope production is undergoing a significant transformation as private investment becomes the primary engine for technical innovation and infrastructure expansion. Unlike the early decades of nuclear medicine which were heavily subsidized by government research budgets, the current era is defined by the entrance of venture capital and large pharmaceutical companies. These entities are increasingly adopting vertical integration models, where a single company manages every step of the process, from the initial irradiation of targets to the final distribution of the therapeutic drug. This approach is designed to streamline the complex logistics and quality control requirements inherent in handling radioactive materials. By controlling the entire chain, these companies can often accelerate the path from production to the hospital bedside, reducing the time-sensitive decay of the isotopes. However, this private-led growth brings new challenges, particularly regarding the long-term sustainability of supply for less profitable but medically necessary isotopes.
The influx of private capital has also sparked a rigorous debate regarding the concept of full cost recovery and its impact on the affordability of advanced cancer care. While the need for a return on investment is undeniable to maintain the pace of innovation, there is a growing concern that the cost of these high-tech therapies could exclude vulnerable patient populations. Policy frameworks must therefore evolve to ensure that market-driven models do not undermine the social imperative of equitable access to medicine. Regulators and industry leaders are searching for a middle ground where sustainable pricing structures can support the expensive infrastructure required for isotope production while ensuring that healthcare systems can afford to integrate these treatments into standard care. Finding this balance is essential for maintaining a stable global market where the drive for profitability and the mission of saving lives can coexist without one compromising the other. This requires a transparent dialogue between the public and private sectors to align financial incentives with global health priorities.
Navigating Systemic and Operational Challenges
Overcoming Logistical Barriers: The Half-Life Race
The production of medical isotopes is only half the battle, as the physical delivery of these materials presents a logistical challenge that is unique in the world of medicine. Because many of the most effective therapeutic isotopes have half-lives measured in days or even hours, the entire supply chain operates under a relentless ticking clock. Any delay in transportation, whether caused by a missed flight, a border crossing issue, or a clerical error, can render a dose completely useless by the time it reaches the patient. The workshop participants identified that the current global logistics network is often ill-equipped to handle the high-volume, just-in-time delivery required for large-scale oncology programs. To solve this, there is a pressing need for the international harmonization of transportation regulations, which would allow radioactive shipments to move through hubs more efficiently. Streamlining these procedures is not merely a matter of convenience; it is a clinical necessity that directly impacts the success rate of the treatments being administered.
In addition to the challenges of delivery, the healthcare infrastructure must also prepare for the significant increase in radioactive waste management that comes with widespread radioligand therapy. Unlike diagnostic procedures that use low-energy isotopes, therapeutic applications involve isotopes that require specialized handling and disposal protocols within the hospital setting. Many existing oncology centers were not designed to manage the volume of waste generated by treating dozens of patients per day with these potent materials. Upgrading these facilities involves significant capital investment in lead-shielded environments, specialized plumbing systems, and long-term storage solutions. Furthermore, the regulatory burden on hospitals to manage this waste can be a deterrent to adopting new therapies. Addressing these downstream bottlenecks is critical; even the most abundant supply of isotopes will fail to improve patient outcomes if the clinical environment cannot safely and efficiently process the materials or manage the resulting waste stream in compliance with environmental safety standards.
Developing Specialized Workforce and Healthcare Pathways
A significant but often overlooked barrier to the security of the isotope supply is the critical shortage of a specialized workforce capable of managing the entire lifecycle of nuclear medicine. From the radiochemists who synthesize the drugs to the nuclear medicine physicians and specialized nurses who administer them, there is a global deficit of trained professionals. This human capital gap threatens to stall the implementation of even the most promising therapies, as hospitals struggle to staff the departments necessary for large-scale rollout. Addressing this shortage requires a concerted effort by educational institutions and governments to create dedicated training programs and certifications. Without a robust pipeline of talent, the industry will remain unable to translate production capacity into actual patient treatments. Investing in the next generation of nuclear scientists and medical professionals is therefore just as vital as investing in reactors or accelerators to ensure the long-term viability of the sector.
The integration of these advanced therapies into standard clinical practice also hinges on the establishment of clear and sustainable reimbursement pathways within national healthcare systems. Because radioligand therapies are often more expensive than traditional chemotherapy or radiation, insurers and government health programs must be convinced of their long-term value and cost-effectiveness. This requires the development of standardized protocols that demonstrate how these precision treatments can reduce overall healthcare costs by improving patient outcomes and reducing the need for prolonged hospital stays. The global community must work toward a consensus on how to evaluate the economic impact of these therapies to ensure that reimbursement models reflect the complexity of the isotope supply chain. By creating a predictable financial environment, healthcare providers can confidently invest in the necessary infrastructure and staff, knowing that the treatments will be accessible to their patients. This alignment between clinical efficacy and financial policy was recognized as a final, essential step in securing the global future of nuclear medicine.
The international community took decisive steps toward a more resilient isotope ecosystem by fostering collaboration across traditionally siloed sectors. The stakeholders engaged in the workshop reached a consensus that the transition from a research-focused field to a global industrial standard required a complete overhaul of existing logistics and production strategies. The discussions concluded that the primary responsibility for this evolution rested on the synchronized efforts of government regulators, private investors, and clinical providers. Experts recognized that previous disruptions in the supply chain were preventable through better data sharing and the harmonization of reactor maintenance schedules. By formalizing these communication channels, the industry moved away from reactive crisis management toward a proactive model of stability. The focus shifted toward creating actionable policy frameworks that addressed both the technical hurdles of isotope production and the administrative barriers to international trade. These efforts established a foundation for a reliable global network that prioritized patient access above all else. This strategic realignment ensured that the remarkable scientific breakthroughs in nuclear medicine were matched by an equally sophisticated and dependable delivery system.