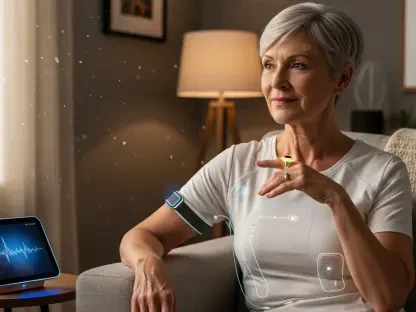The healthcare landscape is currently experiencing a profound structural shift as wearable devices evolve from passive data collectors into sophisticated diagnostic tools powered by artificial intelligence. In the early stages of wearable development, physicians were often overwhelmed by massive streams of raw physiological data that lacked context, making it nearly impossible to integrate into a standard clinical workflow. Today, the focus has shifted toward the synthesis of this data, where machine learning algorithms filter through the noise to identify clinically significant trends that were previously invisible to the human eye. This technological evolution represents a move away from the traditional, episodic model of care toward a continuous and proactive framework. By analyzing heart rate variability, oxygen saturation, and movement patterns in real time, these devices provide a bridge between the patient’s daily life and the medical clinic, ensuring that health monitoring is no longer restricted to the four walls of a hospital or an annual checkup.
The adoption of AI-enabled wearables is effectively dismantling the reactive “wait-and-see” approach that has long characterized modern medicine. Instead of treating a patient only after a symptom becomes severe enough to warrant a visit, clinicians can now rely on automated systems that flag subtle physiological shifts before they manifest as a crisis. This shift toward preventive care is supported by the ability of AI to learn a user’s unique baseline, allowing the software to distinguish between a temporary spike in stress and a genuine medical emergency. As these systems become more integrated into the standard of care, the relationship between the patient and the provider is becoming more fluid. The data no longer sits in a vacuum; it serves as a living record that informs decision-making daily. This constant connectivity ensures that interventions are timely, precise, and tailored to the specific needs of the individual, ultimately reducing the burden on emergency services and improving long-term outcomes for those living with chronic conditions.
The Power of Real-Time Processing
The rapid advancement of edge computing serves as the primary engine driving the current transformation of wearable medical technology across the globe. Unlike traditional systems that require data to be sent to a distant cloud server for analysis, edge computing allows complex mathematical processing to occur directly on the device’s internal microchip. This capability is essential for critical health monitoring because it eliminates the latency associated with data transmission, providing immediate feedback when a life-threatening anomaly is detected. For instance, a wearable ECG monitor can now analyze a heart rhythm locally and alert the wearer to signs of atrial fibrillation within seconds. By handling the analytical heavy lifting at the “edge” of the network, these devices ensure that privacy is maintained and that critical alerts are not delayed by poor internet connectivity. This localized intelligence makes wearables more resilient and reliable in high-stakes medical scenarios where every second counts for the patient.
Modern medical wearables have achieved a level of hardware efficiency that was considered technically impossible just a few years ago. Engineers are now focusing on creating “lean” AI models that require minimal processing power, which extends the battery life of devices and makes them more practical for long-term use. The bulky, intrusive equipment that once defined remote monitoring has been replaced by streamlined sensors that utilize low-energy Bluetooth technology to sync seamlessly with smartphones and tablets. This evolution is particularly significant for bridging the digital divide in rural or underserved areas where high-speed infrastructure may be lacking. Because these devices do not rely on constant high-bandwidth connections to function, they offer a democratic solution to healthcare access. Patients in remote regions can now receive the same level of sophisticated monitoring as those living in urban centers, as the device itself possesses the necessary intelligence to process and store vital health metrics until a basic connection becomes available.
Replacing Snapshots with Continuous Context
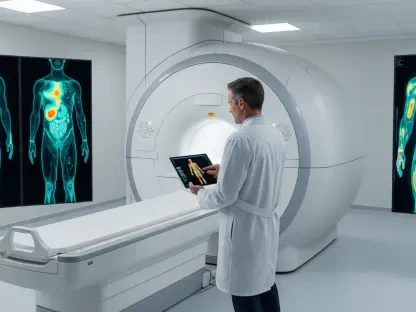
A traditional clinical consultation is frequently compared to a movie trailer because it offers only a brief, curated glimpse into a patient’s overall health status. When a patient sits in an exam room, their blood pressure or heart rate might be temporarily elevated due to stress, a phenomenon known as white-coat syndrome, which can lead to inaccurate conclusions. AI-powered wearables solve this problem by providing the “full feature film” through the continuous tracking of activity, sleep cycles, and various physiological markers over weeks or months. This longitudinal perspective gives clinicians a comprehensive view of a patient’s daily existence, revealing how lifestyle choices and environmental factors interact with their underlying biology. With this depth of information, doctors can move beyond generic advice and develop highly personalized treatment plans that account for the unique rhythms of a patient’s life. This context is invaluable for managing complex diseases where symptoms often fluctuate unpredictably outside the clinic.
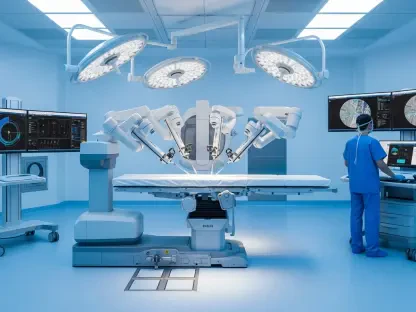
In specialized fields such as physiotherapy and rehabilitation, the integration of AI has revolutionized the speed and accuracy of physical assessments. Previously, a specialist would have to spend hours manually recording and analyzing a patient’s gait or range of motion to track the progress of a recovery plan. Today, wearable sensors equipped with computer vision and motion-sensing algorithms can perform these tasks instantly, providing a level of precision that exceeds manual observation. These systems can detect micro-deviations in a person’s walking pattern that might indicate an increased risk of falling or a failure in a post-surgical implant. By synthesizing data from clinical research databases and consumer-grade sensors, AI models can offer real-time therapeutic guidance that adjusts automatically as the patient grows stronger. This adaptive approach ensures that the rehabilitation process is always optimized for the patient’s current physical state, reducing the likelihood of reinjury and significantly shortening the overall time required for a full recovery.
Expanding the Reach of Specialized Medicine
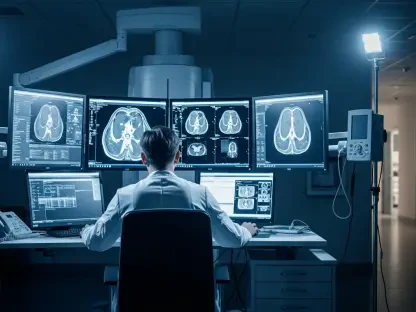
The impact of artificial intelligence in the wearable space is most visible in the burgeoning fields of sleep medicine and neurological health. Sleep is no longer viewed simply as a period of rest but as a critical window into cardiac and cognitive function, with AI models now capable of identifying early markers of sleep apnea or neurological decline. For patients living in rural areas where access to specialized sleep clinics is virtually non-existent, these wearables serve as a vital lifeline. Furthermore, modern devices are expanding their scope to include environmental monitoring, such as tracking ambient noise levels and air quality. Researchers are using this information to understand how external stressors contribute to long-term brain health and the progression of age-related diseases like dementia. By correlating environmental data with physiological responses, AI can provide a more holistic understanding of why certain conditions worsen in specific settings, allowing for more effective lifestyle interventions.
For individuals managing chronic autoimmune diseases, the ability of AI to detect subtle “flare-ups” through wearable data is a transformative development in disease management. These conditions are notoriously difficult to track because symptoms can be vague and highly variable from day to day. AI algorithms can identify minor increases in skin temperature or changes in heart rate variability that often precede a major symptomatic episode. By catching these changes in their infancy, clinicians can proactively adjust medication dosages or recommend behavioral changes to prevent the condition from escalating. This dynamic approach moves away from the “wait until it breaks” philosophy of medicine, focusing instead on maintaining a steady state of health. This proactive monitoring not only improves the patient’s quality of life but also reduces the financial burden on the healthcare system by preventing costly hospitalizations and intensive treatments that are often required when a flare-up is left unchecked.
Bridging the Gap in Clinical Workflows
While the technical capabilities of AI-powered wearables are impressive, their ultimate success depends on how well they integrate into the complex administrative workflows of modern hospitals. One of the primary barriers to adoption has been the friction caused by fragmented data systems, where doctors are forced to log into multiple proprietary platforms to view a single patient’s information. To address this, the industry is shifting toward unified data pipelines that normalize information from various wearable brands and ingest it directly into Electronic Health Records. This ensures that the insights generated by AI are presented to the clinician in a clear, actionable format within their existing digital workspace. By reducing the cognitive load on healthcare providers, these systems allow doctors to spend less time navigating software and more time engaging with their patients. The goal is to create a seamless ecosystem where wearable data is just as accessible and trusted as a standard lab result.
The integration of AI into the medical field is fundamentally an effort to augment the capabilities of human clinicians rather than replace them. As the global healthcare system faces a persistent shortage of licensed professionals, AI-powered wearables act as a force multiplier, allowing a single care team to monitor a much larger population of patients safely. These tools manage the routine task of data surveillance, alerting the provider only when a patient’s metrics fall outside of a predetermined healthy range. This “management by exception” model ensures that medical attention is directed exactly where it is needed most, maximizing the efficiency of limited clinical resources. By moving the site of care from the expensive hospital setting to the patient’s home, these devices are making high-quality healthcare more sustainable and accessible. This transition represents the final step in a broader movement toward a patient-centered, data-driven medical system that prioritizes long-term wellness and personalized intervention for every individual.
Future Considerations: Scaling Personalized Care
The transformation of healthcare through AI-powered wearables has reached a critical stage where the focus must shift toward standardizing data security and ethical algorithmic transparency. As these devices become more deeply embedded in daily life, the volume of sensitive physiological data being transmitted necessitates the implementation of robust encryption and decentralized storage solutions to protect patient privacy. Moving forward, healthcare organizations should prioritize the development of “explainable AI” models, which allow clinicians to understand exactly why a specific health alert was triggered. This transparency is vital for building trust between the technology, the physician, and the patient. Looking ahead, the next logical step is the widespread adoption of agentic AI interfaces that can autonomously manage device updates and data normalization across entire hospital networks. This will remove the technical burden from clinical staff, allowing the technology to function as a truly ambient layer of the modern care continuum.
The success of the next phase of remote monitoring will depend on the industry’s ability to create a unified standard for data interoperability that transcends individual brand ecosystems. Healthcare providers and technology developers must collaborate to ensure that wearable data is not just collected, but also utilized to drive measurable improvements in population health. This involves moving beyond simple alerts and toward the creation of predictive health scores that can forecast long-term risks with high accuracy. The ultimate takeaway for the medical community is that the integration of AI and wearables is no longer a luxury but a necessity for managing the growing demands of an aging global population. By investing in scalable data pipelines and focusing on user-centric design, the industry can ensure that the benefits of this technology are felt by everyone. The transition to a proactive, continuous care model was a necessary evolution that has finally provided the tools required to treat the whole person in real time.