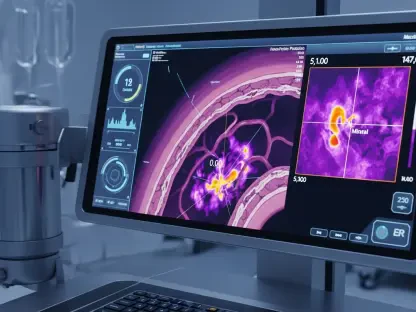
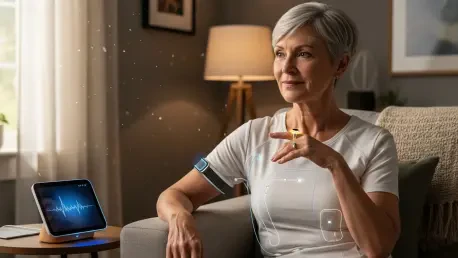The global healthcare landscape is currently undergoing a radical metamorphosis as advanced biometric sensors and artificial intelligence converge to redefine the parameters of patient safety outside traditional clinical settings. Recent data suggests that over sixty percent of chronic disease management now incorporates some form of remote monitoring, a significant leap from the fragmented systems utilized just a few years ago. Historically, wearable devices were viewed primarily as consumer novelties, relegated to the realm of fitness tracking where they provided raw data points—such as step counts or basic pulse rates—that often lacked the clinical context necessary for formal medical intervention. However, the current era has seen these tools evolve into sophisticated medical-grade instruments capable of generating actionable clinical intelligence. This transition marks the birth of a more continuous and proactive model of care that successfully bridges the geographical and socioeconomic gaps between episodic hospital visits and the daily lives of patients, particularly those living in rural or underserved regions where medical resources are often scarce.
From Raw Data to Actionable Clinical Intelligence
The most significant hurdle in traditional remote monitoring was the overwhelming volume of unstructured data, often referred to as digital noise, which made it nearly impossible for clinicians to identify meaningful health trends. In the past, medical professionals lacked the analytical tools required to sift through thousands of heart rate readings or activity logs, leading to missed opportunities for early intervention. Artificial intelligence now serves as a sophisticated filter that autonomously identifies clinically significant patterns, such as early signs of atrial fibrillation or sudden changes in respiratory rate, which might otherwise go unnoticed. This technological advancement allows healthcare providers to shift their focus from the tedious task of manual data entry to the high-value work of personalized treatment planning. By converting a mountain of raw numbers into a clear, prioritized list of medical insights, AI ensures that the care team is alerted only when a patient’s physiological status deviates from their established baseline, thus optimizing resources.
Experts in medical informatics frequently compare a traditional in-person clinical visit to a movie trailer, as it provides only a brief and often incomplete glimpse into the actual health status of a patient. In contrast, AI-enhanced wearables provide the full feature film by capturing physical function and physiological metrics continuously and in real-time. This holistic view is particularly transformative in specialized fields like physical therapy and post-surgical rehabilitation, where AI can analyze a patient’s gait, range of motion, and balance with microscopic precision. These devices integrate multimodal data from various clinical and consumer sources to create a dynamic digital profile that offers therapeutic guidance tailored to the individual’s specific recovery trajectory. This level of customized care was once impossible to achieve outside of a controlled laboratory or clinic setting, but it is now becoming a standard expectation for patients who demand higher levels of autonomy and engagement in their own medical journeys.
Technological Efficiency Through Edge Computing
The technological backbone of the current revolution in remote patient monitoring is the strategic shift toward edge computing, where complex data processing occurs directly on the wearable device rather than in a centralized cloud server. By performing machine learning and predictive analytics locally on the device’s specialized chip, these wearables significantly reduce the amount of energy required for data transmission, thereby extending battery life from days to weeks. This on-device intelligence is not merely a matter of convenience; it is a critical component of sustainability that allows medical hardware to remain functional for longer periods without frequent recharging. Furthermore, processing data at the edge enhances privacy by keeping sensitive biometric information on the person whenever possible. This architecture ensures that high-level predictive alerts are generated instantly, providing the patient with immediate feedback that can be life-saving in acute situations where every second counts.
This fundamental technical shift is also vital for closing the digital divide that has historically prevented equitable access to high-tech medical solutions. Patients residing in remote areas with limited or inconsistent internet connectivity can still benefit from advanced monitoring because the wearable device handles the analytical heavy lifting itself, only transmitting summarized alerts when a connection becomes available. Moreover, the seamless integration of Bluetooth technology into medical implants, such as modern pacemakers and glucose monitors, allows these life-sustaining devices to sync directly with ubiquitous smartphones. This ecosystem eliminates the need for bulky, expensive, and purpose-built home monitoring hardware that often served as a barrier to adoption for elderly or lower-income populations. By leveraging the devices that patients already own, healthcare systems have successfully lowered the barrier to entry, ensuring that constant clinical oversight is a reality for everyone.
Addressing Systemic Challenges and Scalability
For AI-powered wearables to achieve success on a global scale, they must fit seamlessly into the existing daily workflows of physicians and nurses who are already facing unprecedented levels of professional burnout. One of the primary systemic challenges involves data normalization, which is the process of ensuring that information gathered from hundreds of different device manufacturers can be accurately read and interpreted by a single hospital system. Modern healthcare organizations are now prioritizing the adoption of unified platforms that can manage various chronic conditions and different device types through a single, streamlined interface. This prevents the fragmentation of care that occurs when staff are forced to navigate dozens of different software tools to find a single patient’s records. By centralizing this data, hospitals can create a more cohesive narrative of patient health, which is essential for making informed decisions in high-pressure environments.
To support healthcare facilities that are struggling with chronic staffing shortages, the industry has rapidly moved toward the implementation of agentic AI interfaces. These sophisticated systems function as autonomous monitoring assistants that can perform software-based updates and conduct preliminary data analysis without requiring specialized technical skills from the medical staff. By automating the ingestion of high-frequency data streams, these AI agents can handle the administrative burden of monitoring, allowing human clinicians to dedicate their time to direct patient interaction and complex problem-solving. This scalability is particularly important for rural hospitals that may not have the budget to hire a dedicated team of data scientists. By simplifying the way health metrics are tracked and analyzed, technology has transitioned from being a potential distraction to a silent partner that enhances the operational efficiency of the entire medical infrastructure.
Clinical Innovations and the Human Element
The scope of AI wearables is currently expanding into highly complex medical fields such as neurology, immunology, and sleep science, where continuous monitoring reveals secrets that episodic testing cannot. Researchers are now utilizing high-resolution sleep data as a sophisticated early warning system for heart conditions and the onset of neurological decline, identifying subtle changes in REM patterns that precede clinical symptoms. In the near future, these wearables will likely incorporate environmental sensors to track air quality, noise pollution, and UV exposure, determining how these external factors impact brain health and the long-term disease burden of an aging population. This proactive approach moves the point of care from the emergency room to the patient’s living room, facilitating medical interventions that happen before a crisis occurs. This strategy not only improves clinical outcomes but also preserves the patient’s dignity by keeping them in their own community.
Despite initial concerns that the rise of automation might replace human practitioners, AI has instead been embraced as a force multiplier that expands the reach and efficacy of the modern clinician. With a persistent global shortage of licensed healthcare providers, these digital tools allow a single doctor to oversee a much larger patient population while maintaining a high standard of personalized care. AI systems summarize daily health data into digestible reports, ensuring that medical teams only need to intervene when a genuine anomaly is detected or when a treatment plan requires adjustment. This synergy between human empathy and machine intelligence ensures that the relationship between the patient and the provider remains central to the experience. By offloading the mechanical tasks of data tracking to AI, the medical community has successfully protected the human element of care, making the entire healthcare process more responsive, data-driven, and effective.
Strategic Implementation for Improved Outcomes
The transition toward a fully integrated remote monitoring ecosystem required a multifaceted strategy that prioritized interoperability and patient-centered design. Medical institutions that successfully navigated this change focused on establishing robust data pipelines that adhered to the latest encryption standards, ensuring that patient trust remained intact throughout the digital transformation. The integration of wearables into electronic health records was achieved through the adoption of open-source frameworks, which allowed for the seamless flow of information between different levels of care. Clinicians who were early adopters of these technologies reported significant reductions in hospital readmission rates, as they were able to adjust medications and lifestyle recommendations in real-time based on the data provided by the devices. This proactive stance effectively shifted the medical focus from treating acute illnesses to maintaining long-term wellness.
The final phase of this evolution involved a shift in how medical success was measured, moving away from volume-based metrics toward value-based outcomes that favored patient longevity and quality of life. Healthcare systems implemented comprehensive training programs for both staff and patients, ensuring that everyone involved understood how to utilize the wearable technology to its full potential. By providing patients with the tools to monitor their own health, organizations empowered individuals to become active participants in their recovery and maintenance. This collaborative approach proved to be the most effective way to manage the rising tide of chronic diseases globally. Ultimately, the lessons learned from the deployment of AI wearables emphasized the importance of flexibility and scalability in modern medicine. The industry recognized that the future of care would be defined by its ability to adapt to the unique needs of every patient, regardless of where they were located.