The Department of Defense faces a monumental challenge in maintaining a cohesive medical record system that spans across disparate global military installations while simultaneously ensuring that every active duty member’s data remains accessible and accurate during transitions. To address these logistical hurdles, the Defense Health Agency has released a significant solicitation for an indefinite delivery, indefinite quantity contract valued at three hundred million dollars to bolster the operational support and global deployment of the MHS GENESIS electronic health record system. This initiative represents a critical juncture in federal health informatics, as it seeks to stabilize and refine a platform that serves as the backbone for medical care across the military’s expansive footprint. By focusing on site preparation and technical integration, the agency aims to rectify existing inefficiencies that have historically plagued large-scale data migrations. The scope of this procurement covers essential commercial services and materials needed for long-term support.
Seamless Integration: Enhancing Interoperability and Care Quality
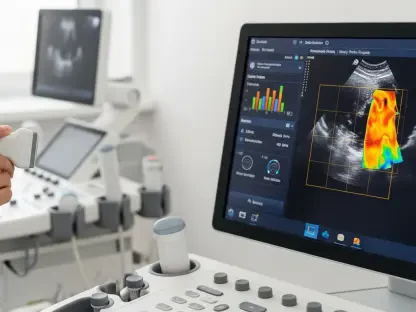
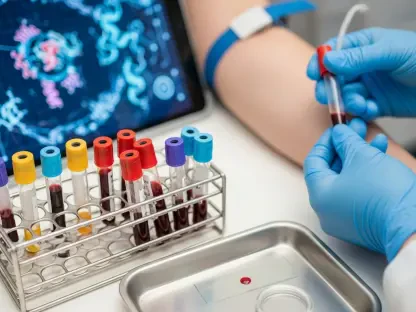
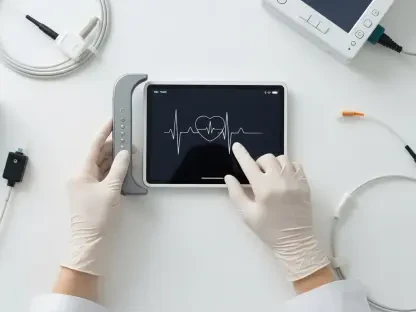
Achieving a unified healthcare experience requires more than just software installation; it demands that every piece of medical equipment, from bedside monitors to diagnostic imaging tools, communicates fluently with a central database. The performance work statement associated with this contract emphasizes the necessity for secure medical device interoperability to protect patient safety and enhance the overall quality of clinical care. While the Department of Defense and the U.S. Coast Guard have successfully reached full deployment across thousands of global locations, the Department of Veterans Affairs has encountered significant technical friction with its transition to the Oracle Health-based platform. This disparity highlights the complexity of synchronizing health data across different administrative structures. The new contract is designed to bridge these gaps by providing robust change management and user training, ensuring that clinicians can focus on patient outcomes rather than struggling with technical barriers. This approach streamlines the flow of critical information between agencies.
To ensure the success of this multi-million dollar investment, federal leadership prioritized the establishment of rigorous technical standards and vendor accountability throughout the rollout process. The procurement structure, which included a base year followed by several one-year options, allowed the government to maintain flexibility in a rapidly evolving technological landscape. Proposers submitted their plans by April 15, marking a transition from planning to active implementation of enhanced data synchronization. Moving forward, the Defense Health Agency focused on creating a feedback loop where frontline medical staff influenced system updates to prevent clinical workflow disruptions. Authorities integrated advanced cybersecurity protocols to safeguard sensitive patient information against emerging threats during the integration phase. These actions paved the way for a more resilient federal health IT ecosystem that prioritized veteran and active-duty health outcomes. Future considerations should involve expanding these interoperability standards to private sector partners who provide care.