The traditional health delivery framework is currently undergoing a radical transformation as the historical disparity between advanced urban medical hubs and isolated rural communities reaches a critical juncture. While residents in metropolitan centers enjoy immediate access to specialized facilities and cutting-edge treatments, those living in remote regions often find themselves trapped in a cycle of systemic neglect. This geographic isolation is exacerbated by a lack of basic infrastructure, a chronic shortage of trained medical professionals, and significant budgetary constraints that prevent the establishment of permanent clinics. Consequently, the necessity for a flexible, technology-enabled approach has never been more apparent than in the current landscape. Virtual care is now emerging as the most viable mechanism to dismantle these long-standing barriers by transitioning from a rigid, facility-centric model to a fluid, patient-centric system. By prioritizing the needs of the individual over the convenience of the institution, digital health is redefining the boundaries of equity.
The Fundamental Shift Toward Patient-Centric Models
The core philosophy of virtual care revolves around the idea that medical expertise should be a mobile commodity rather than a stationary destination for the patient. Historically, the burden of access rested entirely on the shoulders of the individual, who frequently endured long travel times and prohibitive costs to receive even basic consultations. In the current environment, digital platforms are flipping this dynamic by bringing specialized clinical knowledge directly into the homes of underserved populations through synchronous video and asynchronous data sharing. This shift reduces the logistical friction that once prevented patients from seeking timely help, thereby decreasing the likelihood of conditions progressing to advanced stages. As health systems integrate these virtual pathways, the focus moves toward maintaining wellness within the community setting. This evolution ensures that proximity to a physical hospital is no longer the primary determinant of a person’s long-term health outcomes or life expectancy.
Beyond the logistical convenience, the transition to virtual models offers a sustainable solution to the global shortage of healthcare workers by maximizing existing human resources. In rural areas where a single general practitioner might be responsible for thousands of residents, virtual care allows for a more efficient distribution of specialized labor. Physicians can consult with multiple patients across vast distances without the downtime associated with physical transit or the administrative bottlenecks of traditional office visits. Moreover, this model supports the continuous management of chronic diseases such as diabetes and hypertension, which require frequent monitoring rather than intensive surgical intervention. By utilizing digital dashboards and automated notification systems, providers can oversee large patient panels with a level of precision that was previously impossible. This proactive management style not only improves individual health metrics but also reduces the financial strain on public health systems by minimizing emergency room visits.
Technological Pillars of Modern Virtual Infrastructure
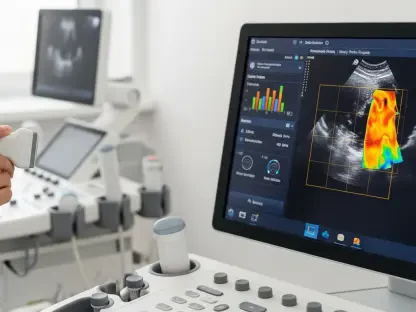
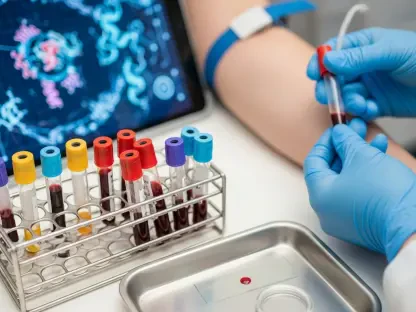
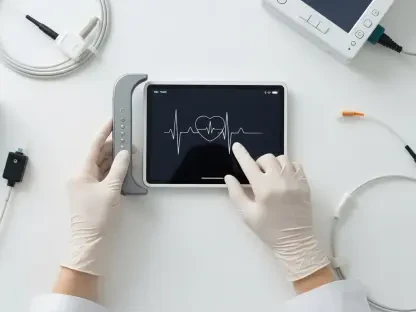
The technological backbone of modern care consists of a sophisticated ecosystem of remote patient monitoring tools and wearable devices that provide continuous data streams to clinicians. Unlike the traditional episodic model of medicine, where a doctor only sees a patient during a scheduled appointment, remote monitoring allows for the real-time tracking of vital signs such as heart rate, blood pressure, and glucose levels. This constant flow of information enables a transition from reactive treatments to proactive interventions, where minor fluctuations in health data can trigger a medical response before a crisis occurs. For patients living in geographically isolated regions, these devices act as a constant link to the medical community, providing a sense of security and oversight that was once reserved for those in high-density urban areas. The integration of these tools into daily life has turned the home into an extension of the clinic, fostering a new level of autonomy.
In addition to monitoring hardware, the rise of artificial intelligence and virtual nursing is optimizing the operational efficiency of hospitals and clinics worldwide. AI-powered diagnostic tools are now capable of performing initial symptom triaging, which helps direct patients to the appropriate level of care and prevents local clinics from becoming overwhelmed with routine inquiries. Simultaneously, virtual nursing programs are being deployed to handle essential administrative duties, such as care plan coordination and discharge documentation, from remote locations. This delegation of tasks allows on-site medical staff to dedicate their full attention to the physical needs of their patients, effectively amplifying the capacity of the existing workforce. By automating the more repetitive aspects of healthcare and utilizing remote personnel for logistical support, the system can provide a higher quality of care even in environments where the physical presence of specialists is extremely limited.
Navigating Regional Implementation and Social Impacts
The successful implementation of virtual care in regions like India provides a compelling case study on how digital health can be scaled to serve massive and diverse populations. Through a synergy of government-led initiatives and private-sector innovation, millions of citizens have gained access to teleconsultations that were previously out of reach. These programs have demonstrated that when central policy support is combined with the widespread availability of smartphones and mobile internet, the digital divide begins to shrink significantly. Private startups are further augmenting these efforts by deploying high-tech diagnostics, such as AI-driven radiology, to areas where trained specialists are scarce. This regional success highlights the importance of localized solutions that respect the unique cultural and economic contexts of the population. When technology is adapted to the vernacular and designed for low-bandwidth environments, it becomes a powerful tool for social and medical advancement.
Virtual care is also making significant strides in addressing specialized health needs, particularly in the realms of mental health and long-term behavioral therapy. In many underserved communities, seeking psychological support is often hindered by deep-seated social stigmas and the high costs associated with traveling to specialized urban centers. Secure video platforms and digital therapeutics offer a private, discreet, and accessible alternative that allows patients to receive counseling from the safety of their own homes. This accessibility is vital for ensuring consistency in treatment, which is a primary factor in the successful management of mental health conditions and chronic illnesses. By providing a platform for continuous engagement, virtual care helps patients adhere to their medication schedules and lifestyle changes, ultimately improving their overall quality of life. The ability to connect with a counselor or a dietitian via a mobile app removes the friction that often leads to treatment abandonment.
Overcoming Systemic Barriers through Hybrid Integration
The path toward universal healthcare access still faces several significant obstacles, primarily regarding the digital divide and the security of sensitive patient data. In the most remote regions of the world, a lack of stable internet connectivity remains a major bottleneck that prevents the full deployment of high-quality video consultations and real-time monitoring. Furthermore, as the healthcare system becomes increasingly digitized, the risks associated with data breaches and privacy violations grow more complex, requiring robust cybersecurity frameworks to maintain public trust. Addressing these challenges required a concerted effort from both policymakers and telecommunications providers to expand infrastructure and establish clear regulatory standards for digital health. Leaders in the medical field emphasized that the goal was not to replace physical medicine entirely but to create a cohesive environment where technology and traditional care worked in tandem to support the patient’s journey.
Strategic integration reached its peak through the adoption of a hybrid care model that combined digital efficiency with the essential nature of in-person clinical visits. While virtual platforms managed routine follow-ups and chronic disease monitoring, the physical infrastructure remained dedicated to complex surgeries and diagnostic procedures that required a tactile human touch. Global health organizations focused on improving system interoperability, ensuring that electronic health records could be accessed seamlessly across different platforms and geographic borders. This approach eliminated the fragmented nature of medical history and allowed for a more coordinated response to patient needs. By fostering public-private partnerships, the industry successfully accelerated the deployment of advanced analytics and automated systems. Ultimately, these actions provided a sustainable framework for bridging the gap in medical access, ensuring that high-quality healthcare became a universal standard rather than a regional privilege.