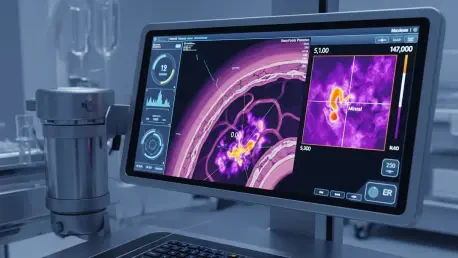
The high-stakes environment of a modern cardiac catheterization laboratory demands split-second decision-making where even a millimeter of error in stent placement can determine a patient’s long-term recovery. For decades, cardiologists relied on the grainy, two-dimensional shadows of traditional angiography, which often obscured the complex, three-dimensional reality of calcified arterial walls and unstable plaques. This diagnostic gap is closing as artificial intelligence integrates with high-resolution imaging to provide a level of clarity that was previously unattainable in real-time clinical settings. Recent regulatory clearances for advanced platforms like the Ultreon 3.0 system signify a pivot toward automated, data-driven vascular care that removes much of the guesswork from complex procedures. By utilizing infrared light to map the internal architecture of the heart, these systems allow for a degree of precision that matches the critical nature of cardiovascular health in the current decade. This evolution ensures that clinicians can see beyond the surface, identifying the exact composition of blockages to tailor interventions specifically to the unique anatomy of every individual patient.
Evolution of Optical Coherence Tomography: Machine Learning Integration
At the heart of this technological leap is the refinement of Optical Coherence Tomography, a modality that uses near-infrared light to generate microscopic-level cross-sectional images of the coronary arteries. While the hardware itself provides the vision, the integration of sophisticated artificial intelligence acts as the brain, instantly interpreting massive amounts of data that would take a human operator much longer to process. The system automatically detects and quantifies calcium deposits, identifies the presence of vulnerable lipid pools, and measures vessel diameters with superhuman accuracy. This automation is vital when dealing with complex lesions where the distinction between different tissue types is subtle but clinically significant. By providing an objective, standardized assessment of the arterial wall, AI-enabled imaging reduces the variability that has historically existed between practitioners. This consistency ensures that every patient receives a high standard of diagnostic scrutiny, regardless of the physician’s individual experience level with intravascular imaging.
Beyond simple identification, the latest iteration of this technology introduces a high-speed, one-second pullback technique that fundamentally changes the safety profile of the procedure. In traditional imaging, the requirement for contrast media to clear the blood from the vessel can pose a risk to patients with compromised renal function, leading to potential kidney injury. The new rapid capture capability allows for extremely fast image acquisition with minimal or even zero contrast media, addressing a major barrier to the widespread adoption of intravascular imaging. This efficiency does not come at the cost of quality; the resulting images remain sharp enough to guide the precise landing zones for stents. By minimizing the physiological stress on the patient, the technology expands the eligibility for advanced imaging to a broader population of high-risk individuals. Moreover, the ability to perform these scans quickly means they can be integrated into the standard workflow without significantly extending the time the patient spends on the operating table.
Advancing Clinical Standards: Implementation and Future Considerations
The broader impact of these advancements is reflected in the growing market confidence and the measurable improvement in procedural success rates within the cardiovascular sector. Since 2026, healthcare systems have increasingly prioritized the acquisition of intelligent diagnostic platforms to bolster their vascular segments, recognizing that the initial investment pays dividends in reduced complication rates and fewer repeat interventions. The automated post-procedure assessment provided by these systems ensures that stents are fully expanded and apposed to the vessel wall, which is the single most important factor in preventing long-term stent failure or thrombosis. This data-driven approach shifts the focus from a purely reactive treatment model to one that is focused on long-term vessel health and optimized blood flow recovery. As clinics adopt these standardized protocols, the reliance on subjective visual estimation is being phased out in favor of a more rigorous, evidence-based methodology that provides definitive answers in the middle of a procedure.
The transition toward AI-driven precision coronary imaging necessitated a significant shift in how interventionalists approached complex arterial repairs and long-term patient management. Medical institutions that successfully integrated these high-speed, automated systems found that they could provide more consistent results while simultaneously protecting patients from the risks associated with excessive contrast exposure. Moving forward, the focus remained on the continuous training of clinical staff to fully leverage the predictive capabilities of these tools, ensuring that the technology was not just an adjunct but a central component of every intervention. Future developments focused on the further fusion of this imaging data with physiological measurements to create a comprehensive digital twin of the patient’s coronary tree. Leaders in the field encouraged the industry to move toward a model where every stenting procedure was guided by these automated insights to eliminate the disparities in care quality. By prioritizing these platforms, the medical community moved toward a reality where interventions were safe.