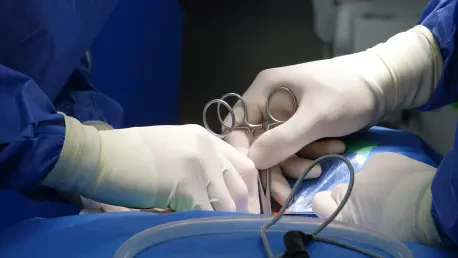
Approximately 1.5 million individuals in the United States currently grapple with the debilitating effects of severe tricuspid regurgitation, a condition that has historically left many patients with few viable recovery options due to the high risks associated with traditional surgery. For decades, the tricuspid valve was frequently referred to by cardiologists as the forgotten valve because the mortality rates for open-heart interventions remained prohibitively high for the elderly and those with multiple comorbidities. This clinical reality created a massive treatment gap, forcing thousands of symptomatic patients to rely on diuretic medications that merely managed fluid buildup rather than addressing the underlying structural failure of the heart. However, the emergence of transcatheter therapies has fundamentally altered this landscape, providing a minimally invasive pathway for surgeons to reach the heart through the femoral vein. By navigating through the vasculature, medical teams can now deploy sophisticated prosthetic valves that restore normal blood flow without the trauma of a sternotomy.
Advancing Clinical Horizons Through Regulatory Success
The Authorization of the TRIVITA Study
The recent decision by the Food and Drug Administration to grant an investigational device exemption marks a definitive turning point for the clinical validation of next-generation transcatheter tricuspid valve replacement systems. This specific regulatory milestone allows for the official commencement of the TRIVITA trial, a pivotal study designed to rigorously evaluate how these artificial valves perform within the complex hemodynamics of the human heart over an extended period. The primary focus of this investigation is to determine if the replacement device can consistently eliminate backflow in patients suffering from symptomatic severe tricuspid regurgitation who are otherwise ineligible for standard surgical procedures. Because the tricuspid orifice is often larger and more irregular in shape than the mitral or aortic valves, the success of this trial depends heavily on the device’s ability to achieve a secure seal and maintain structural integrity against the fluctuating pressures of the right atrium.
Unlike previous early-stage feasibility studies, this pivotal trial is structured to provide the comprehensive data required for a potential pre-market approval, which would eventually lead to widespread commercial availability. The study will enroll participants across a network of premier cardiac centers in the United States, focusing on those whose quality of life has been severely diminished by persistent fatigue and peripheral edema. By establishing clear endpoints for both safety and efficacy, the medical community hopes to confirm that this transcatheter approach not only reduces the mechanical failure of the valve but also significantly lowers the rate of re-hospitalization for heart failure. This transition from experimental status to a formal pivotal trial signals that the technology has reached a level of maturity where it can be tested against the most stringent clinical standards, offering a beacon of hope for patients who have exhausted all other medical avenues in the current year.
Strategic Leadership in the Medical Device Sector
To navigate the complexities of this rigorous clinical phase, the organization has strategically appointed Mike Buck, an experienced executive with a deep history in medical technology, as the new chairman and chief executive officer. This leadership transition is intended to provide the operational expertise necessary to scale manufacturing and ensure that the multi-center trial maintains the highest levels of data integrity and patient safety. Bringing in a leader who has previously guided cardiovascular firms through the transition from research and development to commercialization is a common tactic in the medtech industry, as it provides investors and regulatory bodies with increased confidence in the company’s long-term viability. The new leadership is expected to focus on optimizing the delivery system of the valve, ensuring that interventional cardiologists can deploy the device with high precision and minimal procedural complications during the initial rollout of the TRIVITA study.
Beyond the internal corporate restructuring, this phase of development requires extensive collaboration with multidisciplinary heart teams, which include imaging specialists, interventionalists, and heart failure experts. The success of the trial will depend not only on the mechanical performance of the valve but also on the ability of these teams to accurately screen candidates using advanced echocardiography and computed tomography. As the company moves forward under its new guidance, the focus will likely shift toward streamlining the training protocols for participating clinicians, ensuring that the procedural results are reproducible across different hospital settings. This strategic push is vital for demonstrating that the technology is not just an artisanal solution for elite centers but a scalable standard of care that can be adopted by the broader medical community to treat the growing population of patients suffering from right-sided heart failure and its systemic consequences.
Competition and Technological Evolution in Cardiac Care
Comparing Repair and Replacement Modalities
The competitive landscape for tricuspid interventions is currently divided between two primary philosophies: repairing the existing native valve or replacing it entirely with a prosthetic. For many years, repair devices like the TriClip have been the standard for less severe cases, functioning by clipping the valve leaflets together to reduce the gap through which blood leaks. However, a significant portion of the patient population presents with valves that are too damaged, dilated, or calcified for a simple repair to be effective, which is where replacement systems provide a distinct advantage. By completely substituting the malfunctioning anatomy with a new tri-leaflet valve, replacement technologies offer a more definitive solution that can potentially eliminate regurgitation rather than just reducing it. This distinction is crucial for patients with advanced disease, as even a small amount of residual leakage can lead to continued heart strain and worsening symptoms.
As the industry moves toward 2027, the focus is increasingly shifting toward how these replacement devices can be tailored to the unique anatomy of the tricuspid space, which is characterized by thin walls and a lack of a robust fibrous annulus. Competitive systems like the Edwards Lifesciences Evoque have already paved the way by demonstrating that a replacement valve can be safely anchored even in challenging environments. The entry of new players like VDyne into the pivotal trial stage intensifies this competition, driving further innovation in catheter design and valve materials. This rivalry is beneficial for the healthcare system as a whole, as it accelerates the refinement of delivery systems, making the procedures faster and safer. Clinicians are now looking for devices that offer the lowest possible profile to minimize vascular complications while providing the largest possible effective orifice area to optimize the hemodynamic recovery of the patient’s right ventricle.
Market Dynamics and Future Standards of Care
The medical technology market is currently witnessing an influx of specialized solutions from major players like Medtronic and Abbott, each vying to capture a share of the rapidly expanding tricuspid market. While repair technologies have had a head start, the high demand for replacement systems suggests that the market will eventually support multiple specialized devices catering to different anatomical needs. The presence of several competitors encourages a high standard of clinical evidence, as each firm must prove that its specific design offers superior long-term durability and a lower incidence of common complications such as paravalvular leaks or conduction disturbances. For hospital systems, the availability of various options means they can select the device that best fits the specific pathology of each individual patient, moving away from a one-size-fits-all approach to heart valve therapy.
The medical community previously established that early intervention is key to preventing irreversible damage to the heart and liver, which are often compromised by chronic tricuspid regurgitation. Consequently, the actionable focus for healthcare providers involved the development of robust screening programs to identify candidates for these transcatheter trials before they reached the end-stage of their disease. Clinicians emphasized the importance of integrating advanced 3D imaging into the pre-operative planning process to ensure precise device sizing and placement. Furthermore, hospital administrators moved toward establishing specialized centers of excellence that could handle the unique post-operative needs of this high-risk population. These proactive steps ensured that the transition from clinical trials to standard practice was supported by a well-trained workforce and a sophisticated infrastructure capable of delivering consistent, high-quality outcomes for cardiac patients across the country.