A coalition of fifteen states led by prominent attorneys general recently launched a high-stakes legal battle against the federal government, challenging a radical transformation of the national immunization framework that critics argue compromises pediatric safety for political ends. This legal action, initiated by fourteen attorneys general and the Governor of Pennsylvania, specifically names the Department of Health and Human Services and its leadership, including Secretary Robert F. Kennedy Jr. and acting CDC Director Jay Bhattacharya, as primary defendants in a case that could redefine the boundaries of federal health authority. At the center of the dispute is a sudden and dramatic reduction in the childhood vaccination schedule, which the plaintiffs describe as a reckless abandonment of established scientific standards that have protected the American public for decades. This confrontation marks a historic fracture between state health departments and federal regulators, signaling a period of intense scrutiny over the data-driven foundations of public policy.
Legal Resistance and Institutional Overhaul
The Impact of Administrative Shifts
The legal complaint filed by California Attorney General Rob Bonta and his colleagues focuses heavily on the administrative mechanisms used to implement these sweeping changes to the national immunization schedule. The plaintiffs contend that the dissolution of the original Advisory Committee on Immunization Practices represented a deliberate attempt to silence expert consensus and replace it with a panel of hand-picked skeptics who lack the requisite clinical background. By dismissing the previous committee members before their terms concluded, the administration arguably bypassed the transparency requirements mandated by federal law, leading to what the lawsuit calls an unlawful replacement of a vital scientific body. This restructuring is viewed not merely as a personnel change but as a fundamental shift in how health data is interpreted and disseminated. The states argue that without the oversight of a non-partisan expert panel, the credibility of the Centers for Disease Control and Prevention suffers irreparable damage, leaving local health officials in a precarious position.
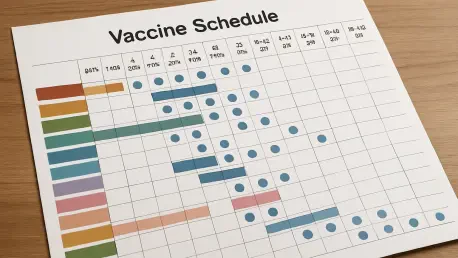
Beyond the procedural arguments, the lawsuit highlights the immediate logistical and financial burdens placed upon state-run healthcare systems as a direct result of the federal policy shift. Attorneys general argue that the reduction of recommended vaccines from seventeen to eleven creates a massive gap in public health coverage that will likely lead to an increase in preventable outbreaks and higher Medicaid expenditures. The legal challenge seeks to restore the original, more comprehensive schedule, asserting that the new directives were issued without the rigorous peer-reviewed evidence traditionally required for such significant modifications. Furthermore, the plaintiffs suggest that the administration’s focus on aligning U.S. policy with specific European models, such as that of Denmark, fails to account for the unique demographic and socioeconomic landscape of the American population. This misalignment, they claim, threatens to destabilize the routine pediatric care protocols that have been refined over years of observation and clinical trials, effectively turning state health departments into experimental grounds.
Policy Divergence and International Comparisons
The shift in federal guidance has sparked a significant rift between government agencies and the broader medical community, with the American Academy of Pediatrics taking the unusual step of issuing its own independent guidelines. Many pediatricians and infectious disease specialists expressed deep concern that the removal of several key immunizations from the universal schedule would lead to a resurgence of diseases that were once considered effectively managed or eradicated in most regions. Medical professionals emphasize that the national immunization framework is designed to create herd immunity, a concept that relies on consistent and high rates of coverage across the entire population. When federal authorities signal a retreat from these standards, it creates a vacuum that is often filled by conflicting advice, leading to parental confusion and decreased compliance at the local level. The tension between political leadership and clinical practitioners highlights a growing crisis in the governance of healthcare, where established expertise is increasingly weighed against populist skepticism.
Institutional dysfunction within the federal health apparatus has further complicated the implementation of the new schedule, with several recent administrative errors resulting in missed legal deadlines for public notification. These procedural failures have forced the postponement of several high-level meetings intended to refine the new recommendations, leading some legal experts to suspect that these delays are strategic maneuvers to evade judicial oversight and public pushback. The lack of a clear and predictable timeline for these policy changes has left schools, insurance providers, and local clinics in a state of uncertainty regarding which vaccines are legally required for enrollment or covered by standard plans. This environment of unpredictability fuels vaccine hesitancy by making the process seem arbitrary rather than scientific. Critics point out that when the mechanisms of public health lose their transparency, the public’s willingness to participate in collective health measures diminishes, which can have long-term consequences for the resilience of the nation’s healthcare infrastructure.
Public Health Implications and Systemic Stability
Erosion of Trust and Clinical Uncertainty
Concerns over public safety and institutional credibility are driving a movement among local healthcare providers to bypass federal recommendations in favor of more conservative, evidence-based practices. California Attorney General Rob Bonta and other plaintiffs argue that undermining the established schedule will drive up infectious disease rates, increase Medicaid costs, and fuel vaccine hesitancy through misinformation. This legal challenge is part of a broader trend of resistance from the medical community, as organizations like the American Academy of Pediatrics have already issued their own guidelines that adhere to the original, more comprehensive schedule. The disconnect between federal mandates and clinical reality creates a fragmented landscape where the quality of pediatric care depends largely on geography. This disparity threatens to deepen existing health inequities, as communities with fewer resources may struggle to navigate the conflicting requirements or secure the necessary vaccines that are no longer supported by federal subsidies or insurance mandates.
The sudden shift in policy also raises critical questions about the long-term economic stability of the healthcare system, as the cost of treating preventable outbreaks far exceeds the price of proactive immunization. Public health experts warned that the administration’s current trajectory poses a direct threat to the welfare of children and the stability of the American healthcare system by ignoring the preventative value of comprehensive vaccination programs. Furthermore, the use of international comparisons to justify the reduction in vaccines has been criticized for ignoring the differences in healthcare access and delivery between the United States and countries like Denmark. In a decentralized system such as that in America, the federal immunization schedule serves as the primary benchmark for schools and employers. Removing these benchmarks without a robust replacement strategy leads to administrative chaos and a loss of public confidence. The ongoing legal battle is thus not just about specific vaccines, but about the fundamental role of government in safeguarding the health of its citizens.
Regulatory Compliance and Future Safeguards
The resolution of this conflict necessitated a renewed focus on reinforcing the autonomy of scientific advisory boards to ensure they remain insulated from the fluctuating tides of political transitions. Legislators and health advocates realized that the current vulnerabilities in the CDC’s appointment process required more robust legal protections to prevent the summary dismissal of expert panels without cause. To mitigate the damage already done, state health departments began developing their own independent data repositories to provide clinicians with the evidence-based resources needed to maintain high standards of care regardless of federal shifts. These decentralized efforts were crucial in maintaining public trust while the legal system adjudicated the limits of executive power over healthcare policy. Educational campaigns were launched to help parents navigate the conflicting information, emphasizing the importance of consulting with primary care providers rather than relying solely on centralized government directives that appeared increasingly influenced by ideological shifts.
Addressing the fallout from these policy changes required a multi-faceted approach involving legislative reform and increased transparency in the decision-making processes of federal health agencies. Health policy experts recommended the implementation of mandatory public comment periods and rigorous peer-review requirements for any major changes to the national immunization schedule. By establishing these safeguards, the system moved toward a more resilient structure that prioritized scientific integrity over political expediency. The states involved in the lawsuit also explored the creation of regional health compacts to standardize vaccination requirements across state lines, ensuring that children remained protected even when federal oversight faltered. Ultimately, the focus shifted toward empowering local communities and medical professionals to lead the way in public health advocacy. These actions served as a vital corrective measure, demonstrating that the preservation of public health depends on a commitment to transparency, evidence-based practice, and the active participation of informed stakeholders.