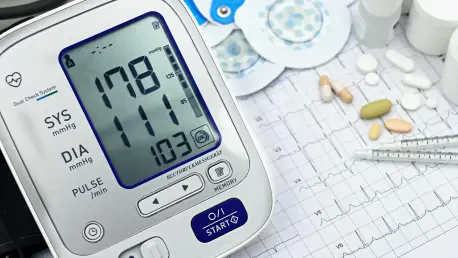
The global prevalence of hypertension has long demanded a diagnostic solution that moves beyond the intermittent and often uncomfortable constraints of traditional pneumatic arm cuffs. KehaAI, a digital health innovator headquartered in Plano, Texas, has officially addressed this need by unveiling the kRing, the first medical-grade wearable device capable of providing continuous blood pressure monitoring without requiring any initial or periodic calibration. This significant technological advancement was introduced by Dr. Vahram Mouradian at the Precision Medicine World Conference in Santa Clara, representing a fundamental shift from recreational fitness trackers to high-fidelity clinical instruments. By eliminating the necessity for a reference cuff measurement, the device removes a primary barrier to long-term user compliance and provides a more accurate reflection of a patient’s cardiovascular health in real-world settings. This launch marks a critical point in the transition toward non-invasive, proactive healthcare that prioritizes both patient comfort and data integrity. The integration of such technology into daily routines allows for the detection of subtle physiological shifts that traditional, infrequent clinical check-ups might overlook.
Redefining Cardiovascular Monitoring Standards: The Calibration Breakthrough
Current smart rings on the market typically rely on photoplethysmography sensors that must be tethered to a traditional cuff for periodic re-calibration, creating a fragmented and often frustrating user experience. The kRing diverges from this standard by utilizing proprietary algorithms and sensor configurations that function independently, ensuring that the blood pressure data remains medically relevant without manual intervention. This innovation is particularly vital for individuals managing chronic conditions like hypertension or hypotension, where consistent data collection is the difference between early intervention and an acute medical emergency. Furthermore, the removal of the calibration requirement allows for more seamless integration into the lives of patients who may find traditional monitoring methods burdensome or difficult to maintain. By focusing on independent operation, the technology provides a reliable stream of physiological metrics that clinicians can trust for diagnostic purposes rather than just general wellness trends. This independence is what separates the device from the saturated market of consumer gadgets that lack the rigor needed for actual medical oversight.
Beyond the software breakthroughs, the physical design of the kRing addresses several mechanical challenges that have previously hindered the accuracy of wearable sensors on the extremities. The patented “ring-with-a-gap” architecture is a deliberate engineering choice that allows the device to expand and contract in response to the natural fluctuations in finger size that occur throughout the day or during sleep. This structural flexibility ensures that the sensors maintain optimal contact with the skin at all times, preventing the signal noise that often plagues rigid wearable designs. Coupled with a battery life that extends for multiple weeks and universal compatibility with modern mobile operating systems, the device is built for the rigors of 24/7 physiological surveillance. Such durability and comfort are essential for capturing longitudinal data, which offers a much more comprehensive view of a patient’s health than a single, isolated reading taken in a clinical environment. By solving the issues of both mechanical fit and sensor stability, the design facilitates a level of continuous monitoring that was previously unattainable in such a small form factor, paving the way for wider clinical adoption.
Strategic Applications: Clinical Utility and Remote Patient Monitoring
The introduction of the kRing facilitates a significant advancement in the field of Remote Patient Monitoring by providing healthcare institutions with high-fidelity, real-time data streams. Institutional providers and clinical researchers can now utilize the device under Institutional Review Board oversight to monitor patient cohorts with unprecedented granularity, especially regarding circadian blood pressure rhythms. These nocturnal patterns are often more predictive of cardiovascular risk than daytime readings, yet they have historically been the most difficult to capture without disturbing the patient’s rest. By offering a non-obtrusive form factor that tracks these variations automatically, the device allows for the identification of “non-dippers” or individuals whose blood pressure does not decrease at night, which is a major indicator of potential heart issues. This level of insight enables a transition from reactive treatments to personalized, precision medicine strategies that are tailored to the specific physiological needs of each patient. Consequently, clinicians were able to monitor patients with a level of detail that traditional methods simply could not provide, leading to more informed and timely medical decisions.
Looking toward the integration of this technology into broader healthcare systems, the potential for reducing hospital readmissions and improving chronic disease management becomes increasingly evident. Healthcare providers were encouraged to adopt these high-fidelity wearables to bridge the gap between office visits and daily life, ensuring that therapeutic adjustments were based on a complete dataset rather than anecdotal evidence. The move toward clinical-grade wearables suggested that the next phase of digital health would focus on interoperability and the seamless transfer of data into electronic health records. By prioritizing medical-grade accuracy and user-centric design, KehaAI established a new benchmark for how cardiovascular health should be monitored in an era where data-driven decisions are paramount. The successful implementation of such devices likely served as a precursor to a more distributed healthcare model where the home serves as a primary site for sophisticated diagnostic and preventative care. As organizations moved forward, the emphasis shifted toward ensuring that patients remained engaged with their own health metrics, ultimately fostering a more proactive and collaborative approach between patients and their specialized care teams.