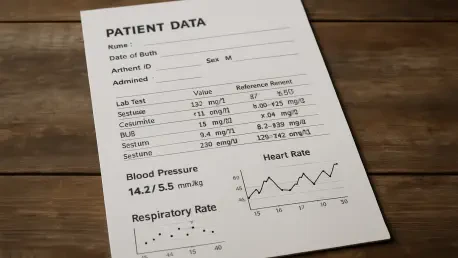
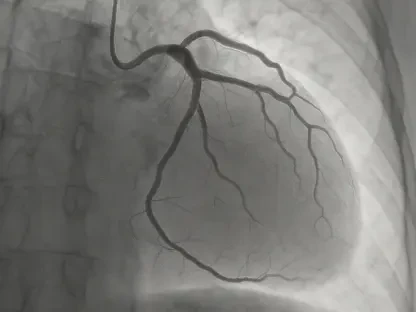
How Is Patient Data Transforming Modern Clinical Workflows?
The healthcare landscape has undergone a seismic shift as clinical teams move away from episodic treatment toward a continuous, data-informed model of population health management. With the rising prominence of value-based care initiatives, modern health systems are increasingly evaluated on their ability to prevent hospital readmissions and maintain patient wellness within the home environment. This transition necessitates a sophisticated integration of Patient-Generated Health Data (PGHD) into existing clinical workflows to ensure that medical intervention occurs before a minor symptom escalates into a crisis. By leveraging real-time streams of information from wearable sensors, mobile applications, and biometric devices, providers are gaining an unprecedented window into the daily lives of their patients. This evolution is not merely a technical upgrade but a fundamental reimagining of the provider-patient relationship, where data acts as the bridge between scheduled visits and the realities of chronic disease management.
Redefining the Patient Experience Through Data Connectivity
Consumer Expectations: The Drive Toward Frictionless Access
Modern healthcare consumers have transitioned from passive recipients of medical instructions to active participants who demand high levels of transparency and convenience. Having grown accustomed to the seamless digital experiences offered by the retail and banking industries, these individuals now expect their healthcare providers to offer similar levels of accessibility and responsiveness through digital platforms. This shift in expectation is driving health systems to adopt mobile-first strategies that prioritize user-friendly interfaces and immediate data feedback loops. When patients can track their own glucose levels, heart rates, or sleep patterns on a smartphone, they naturally expect that information to be available to their medical team in a way that informs their care plan. This demand for “frictionless” interaction is forcing a complete redesign of the front-end patient experience, replacing outdated portals with integrated apps that facilitate two-way communication and real-time health updates effortlessly.
Beyond mere convenience, the active role of the patient in data generation fosters a sense of agency that significantly improves adherence to long-term treatment protocols. When individuals see the immediate impact of lifestyle changes or medication on their biometric data, the motivation to maintain healthy behaviors increases substantially compared to traditional counseling methods. This psychological shift is particularly evident in the management of chronic conditions such as hypertension and diabetes, where daily monitoring is critical for success. Health systems are responding by deploying sophisticated engagement tools, including gamified health challenges and personalized wellness insights driven by the data the patients themselves collect. By meeting patients where they are—on their devices and in their daily routines—providers are effectively extending the clinical environment beyond the four walls of the hospital. This connectivity transforms the patient from a subject of care into a collaborative partner who is equally invested in the outcomes of their health journey.
Proactive Care: Utilizing AI and Real-Time Biometrics
The integration of artificial intelligence and machine learning into the interpretation of Patient-Generated Health Data represents a major leap forward in preventive medicine. Algorithms can now analyze massive datasets from thousands of connected devices to identify subtle patterns that may escape human observation during a standard twenty-minute office visit. For instance, an AI-driven system might detect a gradual trend of decreased physical activity and slight weight gain in a patient with congestive heart failure, signaling fluid retention days before the patient feels any distress. This capability allows clinical teams to move from a reactive posture to a proactive one, where they can reach out to the patient and adjust medication levels before an emergency department visit becomes necessary. The use of these automated monitoring tools ensures that clinicians are alerted only when data points fall outside of customized physiological thresholds, thereby optimizing the use of limited medical resources and focusing attention on the most at-risk individuals.
Furthermore, the application of real-time biometrics is revolutionizing post-operative care and the management of acute recoveries within the community. Instead of keeping a patient in an expensive inpatient bed for observation, hospitals are increasingly utilizing “hospital-at-home” models equipped with advanced sensors that track vital signs around the clock. If a post-surgical patient develops a fever or an abnormal heart rhythm at home, the system immediately triggers a notification to the remote monitoring center, allowing for immediate intervention via telehealth or mobile nurse dispatch. This approach not only reduces the risk of hospital-acquired infections but also significantly lowers the overall cost of care while improving patient satisfaction levels. As these technologies become more refined, the ability to interpret complex biological signals in real-time will become the standard of care for any high-risk medical journey. The goal is no longer just to treat the disease after it manifests but to utilize every byte of patient data to maintain a state of health.
Addressing the Technical and Ethical Challenges of Data Integration
Data Integrity: Managing Volume and Documentation Burdens
While the influx of patient-generated information offers immense clinical value, it also presents significant challenges regarding data volume and the reliability of consumer-grade hardware. Clinicians are often wary of making critical medical decisions based on data from uncertified wearable devices, fearing that inaccuracies could lead to improper treatments or missed diagnoses. To mitigate these risks, health systems are moving toward enterprise-wide standards for data collection, prioritizing devices that have undergone rigorous validation and regulatory clearance. This focus on data integrity is essential for ensuring that information flowing into clinical workflows is actionable and trustworthy. Organizations are also implementing sophisticated data filtering layers that aggregate raw sensor data into meaningful summaries, preventing the “data fatigue” that occurs when providers are overwhelmed by an endless stream of non-critical updates. By curating the data before it reaches the clinician, systems can maintain a focus on high-impact insights.
Another critical hurdle involves the seamless integration of this external data into existing Electronic Health Record (EHR) systems, which were often not originally designed to handle continuous streams of biometric information. If the data is not displayed intuitively within the clinician’s primary workspace, it risks becoming a secondary burden that contributes to burnout rather than relieving it. Current development efforts are focused on creating dynamic dashboards that visualize patient trends over time, rather than just displaying isolated data points. These interfaces must be designed with clinical workflows in mind, allowing doctors and nurses to quickly interpret the significance of the information without navigating away from their standard documentation tools. Effective integration also requires clear protocols regarding who is responsible for monitoring the incoming data and what the expected response times are for various types of alerts. Establishing these operational frameworks is just as important as the technical infrastructure itself in making patient data a functional part of medicine.
Digital Equity: Bridging the Divide in Technology Access
As healthcare becomes increasingly dependent on digital tools and high-speed connectivity, the industry must confront the growing risk of a digital divide that could exacerbate existing health disparities. Patients without reliable internet access, or those who lack the financial means to purchase advanced monitoring devices, may find themselves excluded from the benefits of modern data-driven care models. This concern is particularly acute in rural areas and among socioeconomically disadvantaged populations who often face the highest burden of chronic disease. Health systems are beginning to address this by incorporating social determinants of health into their digital strategies, providing subsidized devices and data plans to those in need. Furthermore, digital literacy training is becoming a standard component of patient education, ensuring that all individuals, regardless of their technical background, can effectively use the tools provided to manage their health and communicate with their medical teams.
Moreover, the design of these digital health tools must be inclusive, accounting for diverse languages, cultural contexts, and varying levels of physical and cognitive ability. A monitoring app that is difficult to navigate or culturally insensitive will fail to engage the very populations that could benefit most from remote monitoring. Developers and clinical advisors are collaborating to create interfaces that are intuitive and accessible to everyone, ensuring that the transition to data-rich care does not leave vulnerable patients behind. By proactively addressing these ethical considerations, the healthcare industry can ensure that technological progress serves as a tool for equity rather than a barrier to access. The ultimate success of these programs will be measured not just by the technological sophistication of the sensors used, but by their ability to reach and improve the lives of all patients, regardless of their personal circumstances. Ensuring universal access to these life-saving technologies is a foundational requirement for modern care.
Future Strategies for Holistic Health Management
The integration of patient-generated data into modern workflows required a fundamental shift in how medical professionals viewed information beyond the clinical setting. Organizations that successfully navigated this transition prioritized the creation of robust data governance policies that balanced the need for real-time insights with the necessity of protecting patient privacy. They moved toward a model where the focus was not on the technology itself, but on the clinical outcomes it enabled, such as reduced readmission rates and improved patient engagement. This transformation was supported by investing in interoperable platforms that allowed data to flow seamlessly between disparate devices and the central electronic health record, ensuring that every member of the care team had access to the same high-quality information. Such initiatives demonstrated that when technology is aligned with clinical goals, it can significantly enhance the efficiency of healthcare delivery while also making care more personalized and responsive to individual needs.
To sustain this progress, health systems recognized the importance of ongoing clinician training and the refinement of automated alert systems to prevent notification overload. They adopted a strategy of continuous evaluation, regularly reviewing the performance of their digital monitoring programs to identify areas for improvement and scale the most successful interventions. Moving forward, the industry took steps to advocate for broader reimbursement models that recognized the value of remote monitoring and preventive data analysis, ensuring the financial viability of these programs. By focusing on scalability and accessibility, providers ensured that the benefits of data-driven care were extended to the broadest possible population. These actions established a blueprint for a more resilient healthcare system that prioritized prevention and patient-centeredness above all else. The journey toward a fully integrated digital health ecosystem showed that the most effective way to manage the health of a population was to listen to the data provided by the patients themselves.