Medical imaging serves as the silent backbone of modern diagnosis, yet the traditional education model often leaves students feeling isolated from the high-pressure reality of a functioning hospital ward. At City College in Santa Barbara, a groundbreaking transformation has turned a once-static classroom into a high-stakes clinical environment where the lines between academic theory and real-world application effectively disappear. This shift is not merely about installing expensive machinery; it represents a fundamental reimagining of how the next generation of healthcare providers interacts with both technology and patients. By replacing outdated, cramped workspaces with a modernized facility that mirrors the layout and workflow of contemporary diagnostic centers, the institution ensures that learners are prepared for the immediate demands of the field. This evolution addresses a critical need in an industry where precision and speed are paramount, and where the transition from a controlled educational setting to a fast-paced medical facility can often be jarring for those who are unprepared for the technical complexities involved.
Integrating Clinical Realism into Academic Curricula
Bridging the Gap: From Textbooks to Phantoms
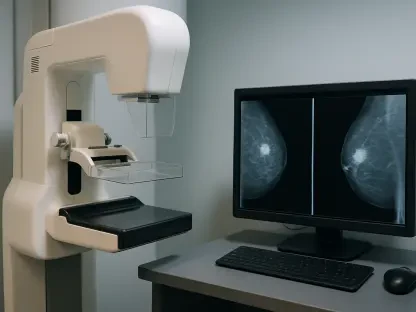
The inauguration of the sophisticated radiology and imaging sciences laboratory marks a significant departure from legacy teaching methods that relied heavily on theoretical instruction. Under the guidance of Program Director Bruce Oda, the newly renovated facility has been meticulously designed to replace inefficient, outdated workspaces with a clinical-grade environment that replicates the exact atmosphere of a modern hospital. This strategic redesign allows students to perform hands-on simulations using radiological phantoms—specialized tools that mimic human tissue—instead of relying on abstract textbook diagrams or static presentations. By working in a space that mirrors professional reality, students can internalize the physical movements and technical nuances required for high-quality imaging long before they step foot into a professional clinic. This immersion is essential for developing the muscle memory and procedural confidence that are often missing in conventional classroom settings, where the gap between theory and practice remains quite wide.
Furthermore, the integration of actual hospital equipment into the lab setting eliminates the “equipment shock” that many new graduates experience during their initial clinical rotations. Instead of learning on simulated interfaces or older hardware that no longer reflects industry standards, students now engage with the same digital imaging systems and diagnostic tools they will encounter in the workforce from 2026 to 2028. This seamless continuity between the laboratory and the clinic ensures that the learning curve is significantly flattened, allowing students to focus on perfecting their technique rather than struggling to understand the basic operations of unfamiliar machinery. By prioritizing a high-fidelity environment, the college is essentially providing a safe space for students to make mistakes, learn from them, and achieve mastery without the pressure of live patient interactions. This proactive approach to education creates a more resilient workforce capable of maintaining high standards of safety and accuracy in any medical setting they might enter after graduation.
Cultivating Professional Identity: The Student-to-Colleague Shift
A core philosophy driving this modernized program is the intentional professionalization of the student experience, moving away from the traditional view of students as mere apprentices. Bruce Oda emphasizes a critical shift in perspective, encouraging faculty and staff to treat learners as future colleagues whose insights and technical skills are already being refined for the professional stage. This approach fosters a sense of accountability and pride that is rarely achieved in standard lecture halls, as it places a heavy emphasis on the nuances of patient-centered care within a high-tech environment. A central component of the current curriculum involves the rigorous cultivation of genuine empathy, which the program carefully distinguishes from mere sympathy. While sympathy might involve feeling sorry for a patient, true empathy requires the technologist to anticipate and respond to the emotional and physical needs of a person in pain or distress, ensuring that the human element remains at the center of diagnostic medicine.
This emphasis on professional identity extends beyond bedside manner to encompass the technical adaptability required in a rapidly evolving field. Assistant Professor Israel Fonseca reinforces this by highlighting the necessity of innovation in a sector increasingly influenced by advanced technologies like artificial intelligence. Students are encouraged to view themselves as lifelong learners who must stay ahead of technological curves, utilizing the laboratory as a testing ground for new ideas and methods. By fostering this mindset, the program ensures that graduates are not just passive operators of machinery but active contributors to the healthcare team who can problem-solve and adapt to new protocols. This cultural shift within the lab environment prepares students for the collaborative nature of modern medicine, where radiologists, technologists, and physicians must work in unison. The lab serves as a microcosm of the healthcare industry, instilling a sense of professional ethics and responsibility that defines their future careers.
Navigating the Technological and Regional Healthcare Landscape
Technological Evolution: Preparing for an AI-Enhanced Future
The current healthcare landscape demands a workforce that is not only proficient in existing technologies but also capable of integrating emerging tools such as artificial intelligence and automated diagnostic software. Within the newly renovated laboratory, the curriculum has been expanded to include simulations that challenge students to work alongside these intelligent systems. This exposure is critical, as AI begins to handle more of the routine image processing tasks, freeing up technologists to focus on more complex aspects of patient care and image optimization. Israel Fonseca notes that the ability to navigate these digital advancements will be a defining characteristic of successful medical professionals in the coming years. By embedding these concepts into the daily lab routine, the college ensures that its graduates are not intimidated by automation but are instead empowered to use it as a tool for enhancing diagnostic accuracy and improving patient outcomes across various clinical environments.
In addition to software integration, the lab emphasizes the importance of hardware versatility and the maintenance of high-quality imaging standards. Students are taught to understand the underlying mechanics of the equipment, ensuring they can troubleshoot minor issues and maintain the integrity of the diagnostic process. This technical depth is essential in 2026, where the reliance on sophisticated imaging has reached unprecedented levels in both emergency and routine medical care. The training ensures that students are prepared for the high-volume environments of regional trauma centers and specialized clinics alike. By providing a comprehensive education that balances manual skill with technological literacy, the laboratory acts as a catalyst for innovation. Graduates emerge with a robust understanding of how to leverage modern tools to reduce radiation exposure and improve the clarity of results, directly impacting the quality of care provided to the community and setting a new benchmark for excellence in the field.
Regional Impact: Meeting the Demand for Skilled Practitioners
Beyond its immediate impact on the student body in Santa Barbara, the laboratory serves as a critical educational hub for a vast three-region area, including San Luis Obispo and Ventura Counties. This regional focus addresses a growing demand for highly skilled medical professionals who can step into entry-level roles with minimal additional training. By providing access to cutting-edge technology and a curriculum that prioritizes clinical excellence, the program acts as a vital pipeline for regional healthcare providers who are often struggling to fill specialized positions. The facility stands as a testament to the college’s commitment to delivering high-quality, industry-relevant education that serves both the students and the broader public. This strategic alignment with regional needs ensures that the investment in the laboratory translates into tangible improvements in community health, as well as providing students with clear pathways to stable and rewarding careers.
The long-term growth of these professionals is a key consideration in the lab’s design, as it provides a foundation that supports career advancement into leadership and specialized roles. Graduates are equipped with the technical proficiency and interpersonal skills required to excel in diverse healthcare settings, from small private practices to large-scale university hospitals. This versatility is increasingly important as the healthcare landscape continues to shift toward integrated, multi-disciplinary care models. By fostering a culture of clinical excellence and human compassion, the program ensures that the transition from the classroom to the professional workforce is as seamless as possible. The facility functions not just as a place of learning, but as a realistic simulation of the modern workforce, ensuring that every student who passes through its doors is prepared to meet the challenges of the future with confidence and skill, ultimately elevating the standard of radiology training.
The implementation of a clinical-grade laboratory at City College successfully bridged the gap between academic theory and the practical demands of the healthcare industry. To maintain this momentum, educational institutions should prioritize ongoing partnerships with local hospitals to ensure that laboratory equipment remains synchronized with the latest medical advancements. Administrators must also consider the regular integration of psychological training modules that focus on empathy and patient communication, recognizing these as core competencies equal to technical proficiency. Future developments should include the expansion of remote diagnostic simulations and the use of cloud-based imaging platforms to prepare students for the increasing prevalence of decentralized healthcare. By continuously updating curricula to reflect the rapid evolution of artificial intelligence and regional healthcare needs, programs can ensure their graduates remain indispensable assets in a shifting medical landscape. Moving forward, the focus must remain on creating immersive learning environments that challenge students to think critically and act with compassion in every clinical interaction.