Despite the significant technological leaps made in modern oncology, geographic barriers and demanding schedules remain the most persistent obstacles preventing women from obtaining life-saving preventative care. In response to these challenges, Mercy Health has launched a sophisticated mobile mammography unit designed to navigate the rural and urban landscapes of Northwest Ohio, bringing clinical-grade diagnostics directly to the doorsteps of local communities. This mobile solution specifically targets a 21-county region, ensuring that individuals who might otherwise skip their annual screenings due to transportation issues or time constraints now have a reliable, high-tech alternative. By deploying a customized vehicle equipped with the same advanced 3D imaging technology found in stationary hospitals, the program effectively eliminates the logistical friction that often leads to delayed diagnoses. These mobile screenings provide women aged 40 and older with a seamless way to maintain their health without the traditional hospital commute.
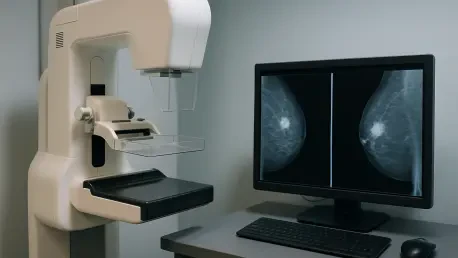
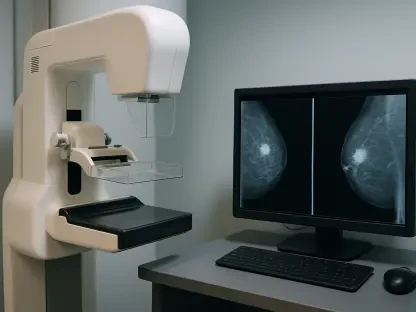
Central to this initiative is the integration of cutting-edge hardware that prioritizes both diagnostic precision and patient comfort, two factors that are historically at odds during breast screenings. The unit features 3D mammography, which provides a series of detailed image slices that allow radiologists to see through dense tissue with greater clarity than traditional 2D scans. Furthermore, a unique patient-controlled self-compression feature addresses the common fear of discomfort by allowing the individual to adjust the pressure once they are correctly positioned by the technician. This sense of agency not only improves the patient experience but also encourages higher compliance rates for future screenings. To ensure that no detail is missed, every scan undergoes a rigorous “double-check” process where certified radiologists review the images alongside computer-aided detection systems. This synthesis of human expertise and algorithmic precision identifies subtle anomalies that might escape the naked eye alone.
Bridging Financial Gaps and Community Reach
Recognizing that the cost of advanced medical imaging can be as much of a deterrent as distance, the program incorporates a robust financial support framework to ensure equitable access for all women. While most insurance providers in 2026 cover 3D mammography as a standard preventative service, the initiative provides specialized “no-cost” programs and financial assistance for those who are uninsured or underinsured. Patients are encouraged to coordinate with Mercy Health – St. Charles Hospital to verify their coverage or seek help managing high deductibles through dedicated assistance lines. The logistics of the rollout are equally comprehensive, with the mobile unit maintaining a rigorous schedule throughout March 2026 across various locations, including Perrysburg, Waterville, and Napoleon. Operating strictly by appointment via the 833-MAMM-VAN system, the unit optimizes throughput while maintaining a personalized environment that mirrors the professional standards of a fixed medical facility.
The implementation of mobile diagnostic fleets successfully shifted the focus of cancer prevention from reactive hospital visits to proactive community-based engagement. Medical authorities observed that by lowering the threshold for entry, participation rates among high-risk populations increased significantly, validating the investment in mobile infrastructure. Moving forward, healthcare systems should prioritize the expansion of these units to include other preventative screenings, such as bone density or cardiovascular assessments, creating a holistic “clinic on wheels” model. Digital integration remained a critical component, and future iterations would benefit from real-time data syncing with centralized electronic health records to streamline follow-up care. Providers who adopted this patient-centric approach found that the combination of accessibility and advanced AI-driven analysis created a more resilient safety net. These efforts established a blueprint for future public health initiatives, demonstrating that the most effective way to fight disease was to meet the patient exactly where they lived.